The error bars are so wide that I think the paper is useless.
3 Likes
We don’t know whether ezetimibe caused the trend towards slightly higher acm or whether high intensity statin usage caused a lower acm compared to combination therapy. If it’s the latter, combined high intensity statin therapy and ezetimibe would yield even better results.
adssx
#453
That’s the whole point of the paper… 
Moderate-intensity statin with ezetimibe combination therapy showed similar cardiovascular benefits to those of high-intensity statin monotherapy
It’s not useless to be able to reach that conclusion.
2 Likes
adssx
#454
Unfortunately, according to this recent paper ( What's the best statin to take? - #440 by adssx ), adding ezetimibe to high-intensity statin seems to yield worse results.
3 Likes
Randy
#455
Is fluvastatin a better bet than crestor due to sirt-6
Activation
1 Like
Simvastatin may be best if you are worried about MS.
Simvastatin (Flolipid, Zocor) is a statin doctors prescribe to treat high cholesterol. It may also help slow down secondary progressive MS. Some studies show that higher cholesterol levels are linked to worsened MS. Because of this, experts thought simvastatin might slow down MS progression if it lowers your cholesterol. But a more recent study found that the drug directly slows down the progression of MS, even if it doesn’t help your cholesterol levels.
Neo
#457
Our results suggest that beneficial effects of simvastatin on reducing the rate of brain atrophy and slowing the deterioration of disability are independent of serum cholesterol reduction.
That might be helpful for aging brains more generally.
Paper:
https://www.pnas.org/doi/10.1073/pnas.1818978116
1 Like
Neo
#458
Only one specific type of MS, but as of Sep 20, this year:
A phase 3 trial revealed that simvastatin, while safe, did not significantly slow disability progression in patients with non-active secondary progressive MS.
However,
However, … , an Italian research team went back to reassess disability levels in 69 participants 8 years later. They found that taking atorvastatin (20 or 40 mg/day) in combination with beta interferon for 2 years in the original study was linked to milder disease progression 8 years later. The researchers suggest that statins may slow down progression in MS, but there may be a lag in the effect. However, this was just a small group from the original study; of the 69 reassessed, 42 had taken beta interferon plus placebo and just 27 had taken beta interferon plus atorvastatin.
Simvastatin | MS Trust.
2 Likes
Wrt. the title of this thread, I’m embarking on an experiment. I’m switching from 10mg/day atorvastatin to 4mg/day pitavastatin. I tolerated the atorvastatin very well for the roughly 5 years I’ve been taking it, but with every passing year, it has been less and less effective at lowering my LDL, best was first year, LDL 70, and worst this year, just got my results, LDL 146. Clearly, I had to do something. My PCP suggested upping the atorvastatin to 20mg/day, but as most of the lipid lowering effect is at the lowest dose, I wasn’t enthusiastic about pushing on the same string. So, I’m going to try a different statin. Monday 10/29 was the last day of my atorvastatin, and I’m taking three days off to allow any trace of atorvastatin to be eliminated, and I’m starting on pitavastatin 4mg/day Friday night. How I will tolerate it, and the impact on my lipid profile ApoB etc., I’ll have to see. There are many comparison studies showing PIT as superior to ATO and other statins wrt. primary MACE endpoints, but found lipoprotein lipase interesting:
3 Likes
Neo
#460
This may be about you as an aging organism more than it about the statin being less effective
(If you wanted to know that you could perhaps consider a 30-60 day washout instead of few days and get your base line normal cholesterol level as of today and compare to when you were younger before starting the first statin)
Above is perhaps less important than just finding what works best for you wherever you are today.
Have you considered adding a second agent? Small amounts of 2-3 agents generally seem to have higher bang per lower side effects.
For instance, do you know if your personal phenotype is cholesterol producer or cholesterol absorber? You can find out for 99 bucks or something like that and if absorber you could have great effects with a small amount of ezetimibe.
3 Likes
Absolutely. Cholesterol levels go up as you age. I’m 66 atm. so very likely my cholesterol went up from 61-66.
And you make many excellent points. Yes, I have considered a multi-drug approach, but it’s complicated. I’m about to embark on adding empagliflozin and rapamycin over the next two-three months, and both of those are known to sometimes raise LDL. My plan was to stick with pita 4mg monotherapy, and assess my lipid profile once all the other drugs were baked in. If at that point my LDL is not at or below 70, I would add bempedoic acid and wait for the effects. If it still does not bring me down to 70 or below, add ezetemibe. PCSK9i is an option, but as a last resort (cost, convenience).
Adding several drugs in small amounts is a valid strategy (as seen in BP control), and if you are a hyperabsorber of cholesterol ezetemibe might be just the ticket. But there is also a signal in a study I can try to dig up, where a monotherapy of high intensity statin was superior in ACM compared to moderate intensity plus eze. So, while sometimes a multi-drug approach is good insofar as fewer side effects with lower individual doses, one has to assess DDI (drug drug interaction). In some cases, you can have synergistic effects, like bempedoic acid and ezetemibe, we must also be aware that more drugs means more interactions which may or may not be beneficial. Furthermore, sometimes the signals can be confusing, as in the medium intensity statin plus ezetemibe being superior to high intensity statin in distinct categories such as plaque progression, but when looked at from an ACM point of view, it is actually inferior. Therefore looking at biomarkers is tricky without taking outcomes into account and especially ACM, plus the longitudinal factor. That is why my plan was to go one drug at a time, then adding another and then another etc. The reason is as outlined above, that with individual drugs the risk/reward profile is better defined - there are plenty of studies showing outcomes for individual statins long term. I know what I’m getting, roughly, on paper. There are dramatically fewer long term studies showing outcomes for drug combinations - again, I say outcomes, as those are superior to just biomarkers.
All these are imperfect of course, but that’s my preliminary approach. I will have to reassess with every intervention. First in line is pitavastatin 4mg/day. Then we’ll see 
1 Like
adssx
#462
You already use atorvastatin, so why not switch to a single-pill combination of atorvastatin and ezetimibe? Same price, not increased pill burden, better safety profile than bempedoic acid.
2 Likes
none really because our bodies need cholesterol. I think people should go by remnant cholesterol not just LDL as a marker for potential heart issues.
True, but I wanted to switch to pitavastatin anyway, as it seems to have superior effectiveness vs MACE events, while having less risk of glucose perturbations compared to atorvastatin, since I’m prediabetic (latest A1c 5.8). Of course there is risk attached, because I really have no idea how I’ll react to pitavastatin, meanwhile I tolerated atorvastatin exceptionally well. Ezetimibe is tricky, since it is commonly accepted to be very safe, perhaps safest among the lipid lowering drugs; I accept that, but I am not satisfied that it provides the best outcomes compared with statins. Longer term trends seem to show statins like atorvastatin to be mildly life extending, but that doesn’t appear to have been shown for ezetemibe, and there may even be a signal to the opposite effect. To be fair, BA has no longitudinal outcome data as yet, while clearly having more side effects compared to ezetemibe, so that’s a valid point. In the end however, there is more doubt in my mind wrt. ezetemibe, because it also depends to a great extent on whether you’re a hyperabsorber or not, and there are still some questions as to how it impacts fatty acid digestion.
It’s a lot of speculation, and ultimately, what matters is how it impacts me specifically, and not what the specs say on paper. So it’s all trial and error.
2 Likes
Neo
#465
Good, thoughtful responses
Please do share
Neo
#466
Can you provide more color on the signal in opposite direction part
Neo
#467
Nowadays very easy and reasonable cheap to check (and don’t have to keep checking a lot of time):
https://empowerdxlab.com/products/product/cholesterol-dx-test?
Fatty acids are best optimized based on testing anyone, omega index, etc, can can also easily be done from home:
https://omegaquant.com/shop/
(I normally do the complete test for 99, but there is a cheaper one for 49h
adssx
#468
Most likely the other way around (for MACE, ACM didn’t reach significance but RR still favours the combination):
2 Likes
adssx
#469
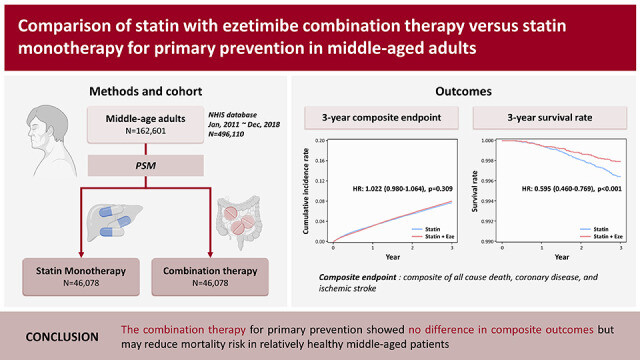
See also: Comparison of Statin With Ezetimibe Combination Therapy Versus Statin Monotherapy for Primary Prevention in Middle-Aged Adults 2024
the 3-year all-cause death rate was lower in the combination therapy group than in the statin monotherapy group (0.2% vs. 0.4%; p<0.001), with a significant HR of 0.595 (95% CI, 0.460–0.769; p<0.001). Single pill combination therapy exhibited consistently lower mortality rates across various subgroups.
Compared to the statin monotherapy, the combination therapy for primary prevention showed no difference in composite outcomes but may reduce mortality risk in relatively healthy middle-aged patients. However, since the study was observational, further randomized clinical trials are needed to confirm these findings.
2 Likes
adssx
#470
Not a lot of evidence for atorvastatin and ezetimibe in terms of life extension (or the opposite): Unraveling Potential Sex‐Specific Effects of Cardiovascular Medications on Longevity Using Mendelian Randomization 2023
For lipid‐lowering drugs, genetically mimicked PCSK9 (proprotein convertase subtilisin/kexin type 9) inhibitors were associated with longer lifespan, particularly in men (2.39 years per SD low‐density lipoprotein cholesterol reduction [95% CI, 0.42–4.36], P for interaction=0.14).
No associations were found for genetically mimicked statins, ezetimibe, or angiotensin‐converting enzyme inhibitors.
Ezetimibe close to statistical significance in men, while statins are on the wrong side for both genders:
4 Likes