Several articles were published this week in the prestigious European Heart Journal on (mostly high-dose) statin monotherapy vs (mostly low-dose) statin + ezetimibe combination (or some variations). I thought a dedicated thread could be useful.
Efficacy of lipid lowering therapy beyond statins to prevent cardiovascular events (Germany)
Treatment with ezetimibe or a PCSK-9 inhibitor was associated with a 19% risk reduction in cardiovascular events (OR [95%CI]: 0.81 [0.75; 0.86]). Effect sizes were similar for myocardial infarction (0.81 [0.74; 0.89]) and even more pronounced for ischemic stroke (0.77 [0.70; 0.84]). In contrast, all-cause mortality was not improved by the intensified lipid lowering therapy (0.99 [0.93; 1.04]). Stratifying by follow-up duration of < vs. ≥ 3 years, no improvement in all-cause mortality was observed in both groups (<3 years: 1.04 [0.93; 1.17]; ≥3 years: 0.97 (0.88; 1.06).
Safety and Efficacy of Moderate-intensity statin plus ezetimibe versus high-intensity statin monotherapy in patients with atherosclerotic cardiovascular disease: a meta-analysis (Brazil)
Analysis revealed significant MIS+EZT-associated with greater percentages in Low Density Lipoprotein (LDL) < 70 (Odds Ratio (OR) 1.76; 95% CI [1.26; 2.45]; p=0.001; I²=73%), LDL reduction (Mean Difference (MD) -5.05 mg/dL; 95% CI [-9.02;-1.07]; p<0.013; I²=56%;); Total Cholesterol reduction (MD -7.91 mg/ dL; 95% CI [-14.90; -0.91]; p<0.027; I²=60%); Triglycerides reduction (MD -8.20 mg/ dL; 95% CI [-13.05; -3.35]; p<0.001; I²=2%;); There was no statistical difference between groups in Drug Adverse reaction (Risk Ratio (RR) 1.19; 95% CI [0.79; 1.78]; p=0.404; I²=0%); and Drug intolerance (RR 0.78 ; 95% CI [0.32; 1.92]; p=0.584; I²=35%).
The upfront lipid-lowering combination therapy of statins and ezetimibe vs statin monotherapy in the reduction of cardiovascular outcomes. A meta-analysis. (US, UK, India, Poland)
Pooled analysis shows that combination LLT significantly reduces the LDL-C level from the baseline (MD, -12.13 mg/dl [0.31 mmol/l] (95%CI: -18.26 to -5.99 mg/dl), p<0.001), all-cause mortality (ACM) (OR, 0.75, 95%CI: 0.62 to 0.92, p=0.01), cardiovascular mortality (CVM) (OR 0.75, 95%CI: 0.66 to 0.84, p<0.001), major adverse cardiovascular events (MACE) (OR, 0.72 95%CI: 0.63 to 0.82, p<0.001), non-significant reduction in the incidence of stroke (OR 0.82, 95%CI: 0.66 to 1.01, p=0.06) when compared with statin monotherapy alone. Similarly, the therapy discontinuation rate was comparable between combination LLT and statin monotherapy groups (OR, 0.87 (95%CI: 0.53 to 1.40), p=0.56). The risk of adverse events related to the gastrointestinal tract (OR, 1.12 (95%CI: 0.93 to 1.36), p=0.23) and musculoskeletal system (OR, 0.88 (95%CI: 0.52 to 1.50), p=0.65) was comparable between both the groups of patients.
Ezetimibe use and mortality after myocardial infarction: a nationwide cohort study (Finland)
Patients with early ezetimibe after MI had lower all-cause mortality during follow-up (33.6% vs. 45.1%; adj. HR 0.77; CI 0.69-0.86; p<0.0001). Early ezetimibe use was associated with lower mortality irrespective of sex, age, atrial fibrillation, diabetes, heart failure, malignancy, revascularization, or statin use. Ongoing ezetimibe therapy during follow-up was associated with lower mortality in time-dependent analysis (adj. HR 0.53; CI 0.48-0.59; p<0.0001).
Efficacy of combination lipid lowering therapy in achieving low density lipoprotein cholesterol targets after one month of event in patients with acute coronary syndrome (India)
dual RE (rosuvastatin plus ezetimibe) and triple REB (rosuvastatin plus ezetimibe and bempedoic acid) combination LLT
The percentage reduction in LDL-C level was 44.4%, 55.5%, and 62.2%, respectively (p<0.001). REB enabled 70.8% and 95.2% of patients to achieve the Lipid Association of India, and American College of Cardiology recommended LDL-C targets of <50 mg/dl and <70 mg/dl within 4 weeks. These target levels were achieved in 67.6% and 88.7% of patients on the dual RE therapy and 50% and 81.6% of patients, respectively, on HIS alone.
Efficacy of combination therapy with statin and ezetimibe versus high dose statin monotherapy in secondary prevention in high-risk patients (Romania)
None of the patients had taken lipid-lowering drugs in the previous 12 months. Patients were randomly assigned to one of two treatment groups: Group 1 - rosuvastatin 40 mg (n= 144) and Group 2 - rosuvastatin 40 mg and ezetimibe 10 mg (n= 120).
As expected, the combination therapy reduced LDL-cholesterol at one month significantly higher compared to high-dose statin monotherapy (-59.65% versus -37.54%; p< 0.0001). After one month of treatment, only 47.92% of patients in Group 1 reached the LDL-cholesterol target (<55 mg/dL) compared to 90.00% of the patients in Group 2 (p<0.0001; R.R.= 0.53).
High intensity statin-ezetimibe combination therapy reduces mortality in patients with ischaemic heart disease and elevated Lipoprotein(a) (Singapore)
Compared with a less intensive regimen, HI statin-ezetimibe was associated with reduced risk of all-cause mortality (HR 0.44 [0.21-0.89], P=0.023) and MACE (HR 0.71 [0.52-0.95], P=0.027), with no statistically significant effect on cardiovascular mortality (HR 0.43, P=0.142). Notably, the cardiovascular benefits of HI statin-ezetimibe were more pronounced in patients with elevated Lp(a); a greater reduction in risk of MACE was seen for patients with Lp(a) ≥70 nmol/L (HR 0.51, P=0.007) or Lp(a) ≥100 nmol/L (HR 0.36, P=0.009), and in all-cause mortality risk for those with Lp(a) ≥70 nmol/L (HR 0.24, P=0.025). Although LDL-C reduction >50% was associated with reduced risk of all-cause mortality (p=0.027), this could not fully explain the overall cardiovascular benefit of HI statin-ezetimibe use in patients with or without elevated Lp(a).
Combination of moderate-intensity statins and ezetimibe versus high-intensity statins alone for primary prevention of cardiovascular events (Canada, US)
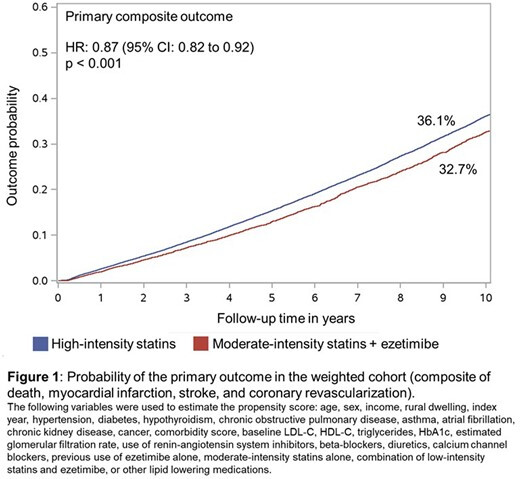
We included all adults aged ≥ 67 years (eligible for drug coverage) with a first prescription of either a combination of moderate-intensity statin with ezetimibe (“combination therapy”) or high-intensity statin alone between January 2010 and December 2022. Patients were excluded if they had not received any prior lipid lowering therapies or had a history of myocardial infarction (MI), stroke, heart failure, peripheral vascular disease or prior coronary revascularisation at any time before or within 3 months of treatment initiation.
The cumulative incidence of the primary outcome at 10 years in the weighted cohort was 32.7% in the combination therapy group and 36.1% in the high-intensity statin group (HR: 0.87; 95% CI: 0.82 to 0.92; p<0.001; absolute risk reduction: 3.5%; 95% CI: 0.8 to 6.1; Figure 1). This result was primarily driven by a lower risk of all-cause death (HR: 0.85; 95% CI: 0.80 to 0.91; p<0.001; Figure 2) and stroke (cause-specific [cs] HR: 0.86; 95% CI 0.74 to 0.99; p=0.04), whereas no differences were observed in the risk of MI (csHR: 0.97; 95% CI: 0.82 to 1.15) or coronary revascularization (csHR: 0.97; 95% CI 0.85 to 1.11).
Moderate-intensity statin combined with ezetimibe versus high-intensity statin monotherapy for secondary cardiovascular risk reduction: a systematic review and meta-analysis (Italy, US, Brazil, Taiwan, India)
Cardiovascular mortality (RR 0.83; CI95% 0.73-0.94; p=0.003), all-cause mortality (RR 0.90; CI95% 0.82-0.98; p=0.02) and non-fatal stroke (RR 0.83; CI95% 0.73-0.93; p=0.002) were significantly lower in patients treated with MIS+EZE compared to those treated with HIS. A significantly higher proportion of patients in the MIS+EZE group reached an LDL-C ≤ 70mg/dL (RR 1.26; CI95% 1.19-1.34; p<0.00001). No statistically significant difference was found for non-fatal myocardial infarction (RR 0.87; CI95% 0.64-1.17; p=0.36), coronary revascularization (RR 1.03; CI95% 0.78-1.35; p=0.83), heart failure (RR 0.95; CI95% 0.86-1.06; p=0.38) and unstable angina (RR 1.52; CI95% 0.62-3.75; p=0.36). A RCT sub-analysis was feasible for cardiovascular mortality and showed no statistically significant difference between the two groups (RR 1.01; CI95% 0.42-2.42; p=0.98).
Regarding safety endpoints, the risk of adverse events (RR 0.84; CI95% 0.74-0.95; p=0.004) and the risk of muscle-related adverse events (RR 0.67; CI95% 0.49-0.92; p=0.01) were significantly lower in MIS+EZE group. The significant reduction in muscle-related adverse events was maintained in the RCT sub-analysis (RR 0.61; CI95% 0.41-0.91; p=0.02). There was no difference between groups in the risk of liver-related adverse events (RR 0.63; CI95% 0.29-1.41; p=0.26) or new-onset malignancy (RR 0.99; CI95% 0.87-1.12; p=0.85).
All the above are from the European Heart Journal, while this one is from a less prestigious journal and research team: Efficacy and safety of double-dose statin monotherapy versus moderate-intensity statin combined with ezetimibe dual therapy in diabetic patients: a systematic review and meta-analysis of randomized controlled trials (India, Pakistan, Bangladesh, Ukraine, US)
Monotherapy showed no significant difference compared with dual therapy for low-density lipoprotein-cholesterol levels [mean difference (MD): −5.03; P = 0.37], high-density lipoprotein-cholesterol levels (MD: 0.01; P = 0.95), total cholesterol (MD: −2.38; P = 0.66), and triglycerides (MD: 5.37; P = 0.67) at follow-up compared to baseline. Monotherapy significantly reduced serious clinical adverse events (risk ratio: 0.21; P = 0.04), with no difference in treatment-related adverse effects, discontinuation due to treatment-related or overall adverse events.
Other similar papers published on this topic this year that reached similar conclusions:
To me, the topic is now closed, and low-dose statin + ezetimibe seems superior to high-dose statin. Thoughts @CronosTempi @Neo @A_User?