A_User
#310
The benefit is exactly the same from decreasing LDL from 60 to 30 as if 100 to 70. Of course from 100 to 30 would have twice the benefit. On longer time scales it would be even higher.
1 Like
L_H
#311
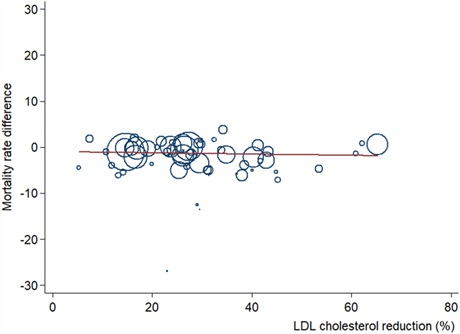
Interesting study that finds against the “lower the better” hypothesis.
This graph seems to encapsulate the key point that lowering ldl-c by more doesn’t translate to mortality benefit.
“WHAT THIS STUDY ADDS
Trials reducing LDL-C more than 50% did not consistently further decrease all-cause and CV mortality; the reduction in MI risk was consistent across all analyses.
Mortality benefits were found within trials with baseline LDL-C levels more than 130 mg/dL.
Achieved LDL-C levels were not related to mortality reductions.”
Interesting that they couldn’t find any benefit if starting ldl-c is already below 130mg/dl.
The idea that lowering apob or ldl-c confers the same benefit no matter where the start point isn’t supported by any intervention studies.
4 Likes
Yes, a 50% LDL reduction seems to have the maximum effect on all cause mortality. That’s taking an LDL of 120 down to 60, which is pretty darn good. I guess it just means that extra mile from 60 to 30 doesn’t really have the bang for the buck.
3 Likes
L_H
#314
Yes, the meta analysis additionally finds this for cv deaths as well as ACM.
“Intensive LDL-C percent lowering did not further reduce CV mortality”
Driving LDL-C to ~60mg/dL and lowering inflammation with intensive statin therapy or dual statin/ezetimibe therapy may drive cardiovascular risk to near 0 even over many decades. Maybe a lifetime clinical trial involving millions of people would find a small, statistically significant acm in the statin+ezetimibe+PCSK9i group compared to the statin+ezetimibe+saline injection group.
If there was a cheap, oral PCSK9i I would add it to my stack but as of now I see no point in paying hundreds of dollars/euros for a monthly injection.
1 Like
adssx
#317
Do we have data on LDL and mortality (all-cause or CV) but for a given total cholesterol?
For instance instead of a 2D plot a 3D one with LDL (or ApoB) as x and Total cholesterol (or HDL) as y and in z mortality.
3 Likes
A_User
#318
Do you have a link to a study showing that there is a attenuation in the decrease in ACM at higher LDL reduction?
Most therapies can’t lower LDL above 50% so of course there isn’t enough data for that. Which reduces the statistical power.
I see that the case that most things said here and I imagine everywhere else is simply false, still holds true.
Absolutely pathetic for people to weaponize a lack of statistical significance like this. It’s dangerous. It’s evil. It’s misinformation. And I guess I have to call it out when I see it.
I have no problem trying to reduce LDL as low as possible. At some point the law of diminishing returns sets in. For me, that means I probably won’t pay the extra additive expense of a PCSK9i as getting to 60 should be sufficient for me. Spending a lot of extra money every month (as well as the inconvenience of an injection) to get a marginal improvement is not worth it for me personally. If others feel differently, that’s OK too. I’d rather skip the PCSK9i and spend $300 a month on other anti-aging treatments - Rapamycin, Empagliflozin, Lithium, etc…
I am using Bempedoic Acid, Ezetimibe and O3 fish oil as well as a healthy(ish) diet to lower my LDL as much as possible. If I could, I’d use a statin as well.
I think you would also agree that you get most of the benefits dropping from a high number (100-150) to a number half that size (50-75) for LDL. Is there a benefit to going lower? Maybe. Is it worth it? Not for me.
4 Likes
A_User
#320
It sounds to me that you gave up and you are happy with having a suboptimal apoB. If that is your decision. I wouldn’t stop at PCSK9i but also look at other ways of lowering apoB further if you care about not getting atherosclerosis or heart disease for sure.
Some are clutching their 10-year risk calculators in one hand, and their magic crystals in the other, and are hoping for the best. I don’t know the difference.
This is interesting, an effect I was not aware of:
Effect of lipid-lowering therapies on C-reactive protein levels: a comprehensive meta-analysis of randomized controlled trials !
“Statins, bempedoic acid, ezetimibe, and omega3FAs significantly reduce serum CRP concentration, independently of LDL-C reductions.”
11 Likes
L_H
#322
Yes, i don’t think there are any intervention studies in primary prevention that suggest you should go lower. The population association studies suggest you shouldn’t go lower, and the Mendelian randomization studie show a small absolute benefit “being” lower from natural genetics. Each type of study has limitations, but it seems that the various limitations of MR studies are the hardest for people to understand.
The idea that we can simply choose to have a lower apob is an obvious fallacy. We would choose an intervention, and that intervention would need to be used long term to bring benefit, and would come with potential side effects. These side effects of targeting vlow levels of apob haven’t been tested over the long term. So the side effects of using say, psk9i to go lower may easily outweigh any small absolute cvd benefits. We just don’t know from the evidence base.
It’s understandable that people fixate on cholesterol when they fear cvd, because it gives them a sense of control, but in reality death is a multi-factoral disease and longevity requires a multi-factoral approach. Even having your apob down at 30 doesn’t eliminate cvd risk. And if it comes at the expense of minor sarcopenia or minor mitochondrial impairment then the tradeoff may not be worth it.
3 Likes
L_H
#323
This is an area I’m very interested in. The idea that statin benefits come from 2 mechanisms is intriguing. And I’m fascinated by the size of the bempedoic acid impact.
Does anyone know of any studies which show the dose response curve for statins on crp?
3 Likes
adssx
#324
I assume that the slight (and not statistically significant) increase of CRP concentration for CETP inhibitors is based on the trials of failed CETPi? Did they report CRP in obicetrapib trials?
@A_User as you’re our lipid expert, do you have any thoughts on this by any chance: What's the best statin to take? - #317 by adssx ?
1 Like
A_User
#325
HDL can be atherogenic at high levels iirc. If you substract HDL from total cholesterol you get the mass of all the atherogenic apoB particles, and it is also predictive in a different way, said as non-HDL-c. So amount of apoB particles matter but also the mass of them. I haven’t seen such 3D graph iirc but it would be interesting to see. HDL doesn’t do anything for ASCVD as there have been numerous CETPi that have failed and they pretty much only raised HDL. The only one with some effect decreased LDL as well but they didn’t bring it to market. The new CETPi decreases LDL by a lot too.
1 Like
adssx
#326
Thanks. Yes, I wonder whether “the lower the better” for ApoB could be correct as long as, for instance, your total cholesterol doesn’t go below a certain threshold (and isn’t too high either). Anyway, the obicetrapib and obicetrapib/ezetimibe trials might indirectly answer this question. Can’t wait to have the results.
4 Likes
L_H
#327
On the HDL point. This gives a good overview on how and when hdl is antiatherogenic. I’d love to see something more recent
The metabolism and anti-atherogenic properties of HDL - PMC.
" The best known of these is their ability to remove cholesterol from cells, such as macrophages in the artery wall, in the first step of the reverse cholesterol transport pathway (5). HDL also inhibit LDL oxidation (6), promote endothelial repair (7), improve endothelial function (8), have anti-thrombotic and anti-inflammatory properties (8, 9), and inhibit the binding of monocytes to the endothelium (10). In addition to preventing atherosclerotic lesion progression, HDL also promote lesion regression in animals"
1 Like
adssx
#328
Gilles Lambert, co-author of this 2009 (!) paper published this in 2023: HDL as a Treatment Target: Should We Abandon This Idea?
High-density lipoproteins (HDL) have long been regarded as an antiatherogenic […] Unfortunately, neither increasing HDL with drugs nor direct infusions of reconstituted HDL have convincedly proven to be positive strategies for cardiovascular health, raising the question of whether we should abandon the idea of considering HDL as a treatment target. […] The results of two large clinical trials, one testing the latest CETP inhibitor Obicetrapib and the other testing the infusion of patients post-acute coronary events with reconstituted HDL, are still awaited. If they prove negative, these trials will seal the fate of HDL as a direct therapeutic target. However, using HDL as a therapeutic agent still holds promise if we manage to optimize their beneficial properties for not only ASCVD but also outside the cardiovascular field.
Lambert’s 2009 paper is also cited in this 2023 Iranian paper: HDL-cholesterol concentration and its association with coronary artery calcification: a systematic review and meta-analysis
According to this analysis of observational studies, high HDL-C levels were not found to predict protection against CAC. These results suggest HDL quality rather than HDL quantity is important for certain aspects of atherogenesis and CAC.
Interestingly, some observational clinical studies have indicated an association between different HDL subfractions and CAC. […] In a cross-sectional study, HDL-P and medium size HDL-P were protective against CAC (OR: 0.42 (0.22, 0.79), 0.002 and 0.36 (0.19, 0.69), 0.006, respectively), while large HDL-P and average size HDL-P were not (OR: 0.77(0.33, 1.83), 0.29 and 0.72(0.35, 1.48), 0.58, respectively).
HDL size is also a determinant of the anti-atherogenic properties of HDL. […] In another cross-sectional of Healthy Women Study, large HDL was inversely associated with CAC, but small HDL was not.
Thus, there is a controversy between the results of HDL particles and subfractions with CAC. This is probably due to the absence of a unique gold standard to measure the functional and physical characteristics of HDL subfractions among studies. Lack of standard and easily applicable methods to analyze and detect HDL particles and subfractions, limits their clinical usefulness for the assessment of cardiovascular risk. Therefore, further studies are needed to fully understand the impact of HDL subfractions and HDL-C in atherosclerotic CVD risk stratification in para clinics and different populations
3 Likes
L_H
#329
Yes that’s very interesting, quality not quantity may be the critical thing.
It got me wondering whether there are any MR studies on this. There are genetics associated with higher hdl, so you’d expect to see some papers.
All I’ve found so far relates to infection, not cvd.
“Mendelian randomization using genetic variants associated with HDL-C as an instrumental variable was consistent with a causal relationship between elevated HDL-C and reduced risk of infectious hospitalizations”
https://www.ahajournals.org/doi/10.1161/ATVBAHA.119.313381#:~:text=Mendelian%20randomization%20using%20genetic%20variants,method%2C%20P%3D0.001).
L_H
#330
Found a recentish paper
https://www.metabolismjournal.com/article/S0026-0495(20)30215-8/fulltext
Results
Genetically determined HDL cholesterol and apolipoprotein A-I levels were not associated with CAD.
HDL mean diameter (β = 0.27 [95%CI = 0.19; 0.35]), cholesterol levels in very large HDLs (β = 0.29 [95%CI = 0.17; 0.40]), and triglyceride content in very large HDLs (β = 0.14 [95%CI = 0.040; 0.25]) were directly associated with CAD risk, whereas the cholesterol content in medium-sized HDLs (β = −0.076 [95%CI = -0.10; −0.052]) was inversely related to this risk.
1 Like
Neo
#331
@L_H @scta123 you’ve both in the past asked for my perspective / why I weigh going after Apo B in an aggressive way. This paper hits many of those reasons so I thought I’d share it.
There is urgent need to treat atherosclerotic cardiovascular disease risk earlier, more intensively, and with greater precision: A review of current practice and recommendations for improved effectiveness
The relationship between low-density lipoprotein cholesterol (LDL-C) and risk for ASCVD is one of the most highly established and investigated issues in the entirety of modern medicine. Elevated LDL-C is a necessary condition for atherogenesis induction. Basic scientific investigation, prospective longitudinal cohorts, and randomized clinical trials have all validated this association. Yet despite the enormous number of clinical trials which support the need for reducing the burden of atherogenic lipoprotein in blood, the percentage of high and very high-risk patients who achieve risk stratified LDL-C target reductions is low and has remained low for the last thirty years. Atherosclerosis is a preventable disease. As clinicians, the time has come for us to take primordial and primary prevention more serously. Despite a plethora of therapeutic approaches, the large majority of patients at risk for ASCVD are poorly or inadequately treated, leaving them vulnerable to disease progression, acute cardiovascular events, and poor aging due to loss of function in multiple visceral organs. Herein we discuss the need to greatly intensify efforts to reduce risk, decrease disease burden, and provide more comprehensive and earlier risk assessment to optimally prevent ASCVD and its complications. Evidence is presented to support that treatment should aim for far lower goals in cholesterol management, should take into account many more factors than commonly employed today and should begin significantly earlier in life.
https://www.sciencedirect.com/science/article/pii/S2666667722000551
Can be paired with this figure that Tom Dayspring recently tweeted
7 Likes