I haven’t seen this discussed anywhere on the forum, but here is another intervention that significantly impacts mice lifespan:
Counteracting age-related VEGF signaling insufficiency promotes healthy aging and extends life span
Do you think there are any implications for humans? Are you doing anything personally? Interestingly, many interventions are targeted at inhibiting VEGF and angiogenesis.
What are some ways to improve signaling? There is, of course, cardiovascular training, but I’m sure there is more.
One food that seems to increase VEGF is wakame (brown seaweed), also known as undaria pinnatifida:
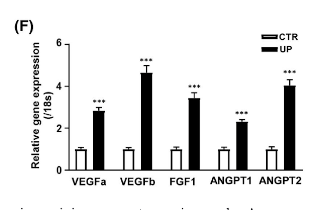
4 Likes
So if VEGF increase lifespan and is not something to fear speciality related to cancer, in this case the fears related to BPC 157 use would be minimized?
Curious
#5
This is an amazing presentation of the Vascular theory of aging.
How normalizing a youthful expression of VEGF reduces cancer, improves the number of stem cells, improves muscle function, decreases fat deposits, makes the thymus age more slowly and so on. It increases lifespan and, at the same time, compresses age-related morbidity.
Amazing!
4 Likes
Curious
#6
Another great ARDD talk which highlights, among many other things the importance of the microvascular aging for brain health and lots of other useful information, for instance about GLP 1 receptor agonists for brain health.
At around 12,45 minutes, he talks about that neurologists historically have focused on imaging the macro vascular and the diseases in the big arteries and screaing for vascular risk factors, but not been focused on the 500 miles of microvascular system in the brain. (500 miles is his figure, not mine). A micro vascular system that supplies all brain tissues with blood and oxygen. It is the microvascular system that penetrates the white matter in the brain, a white matter that gets degenerative spots of over the life course and which often are neglected, because they are seen as a normal part of aging, “aging-spots”
Decreased perfusion-pressure of the brain and the resulting decreased oxygen and blood flow makes the brain overexpress amyloid. A decreased perfusion also changes how amyloid precursors are cleaved. In a hypoxia-situation less precursors to amyloid are cleaved and therefore amyloid is built up in the brain, and less amyloid is also “disposed” from the brain.
In a situation with normal supply of oxygen, more precursors to amyloid are cleaved, and therefore less amyloid is produced.
At 26,30 he talks about the gero-therapeutics that are in randomized placebo-controlled trials for preclinical Alzheimer’s/dementia. There are ongoing trails with SGLT2 inhibitors, Metformin, GLP 1 receptor agonists and Rapamycin.
I did not know that GLP 1 is a neurotransmitter in the brain. And at 27,30 we enter a phase in the talk that is almost a hallelujah for GLP 1 receptor agonists. He talks about how:
- They reduce the expression of amyloid and Tau.
- They increase the clearance of amyloid and tau.
- They reduce neuroinflammation.
- They improve insulin sensitivity
- They reduce oxidative stress
- They increase neurogenesis in the hippocampus
- They improve synaptic plasticity.
GLP 1’s not only reduce the risk factors, but they can also be seen as a directly neuroprotective class of medications, which he think should be prescribed off label to people with some risk of developing dementia /Alzheimer’s. .
3 Likes
Have you tried this wakame extract? The results are extremely positive in that study.
Exercise
From angio.org
Exercise builds muscle, and to do this, it stimulates growth factors to increase in the bloodstream, and these growth factors not only provides an expanded blood supply to support enlargement of the muscle itself, but the factors also attract angiogenic stem cells that normally reside in the bone marrow to enter the circulation and home in on growing muscle. These stem cells build both muscle and the blood vessels required to supply it. Exercise also increases angiogenesis in the lung and brain. Regular exercise is important for health.
References:
Bonsignore MR, Morici G, Riccioni R, et. al. Hemopoietic and angiogenetic progenitors in healthy athletes: different responses to endurance and maximal exercise. J Appl Physiol. 2010 Jul;109(1):60-7.
Möbius-Winkler S, Hilberg T, Menzel K, et. al. Time-dependent mobilization of circulating progenitor cells during strenuous exercise in healthy individuals. Appl Physiol. 2009 Dec;107(6):1943-50.
Tang K, Xia FC, Wagner PD, Breen EC. Exercise-induced VEGF transcriptional activation in brain, lung and skeletal muscle. Respir Physiol Neurobiol. 2010 Jan 31;170(1):16-22.
1 Like
Curious
#9
Thank you for sharing. I did not know that angio.org existed. Yes, exercise is the first intervention that comes to mind for improving brain health, as is healthy Sleep.
Besides those, I wonder what interventions, that right now, can be used as interventions with meaningful effects on the micro-vasculature. There are lots of supplements that have been proposed to increase circulation in the brain. Lutein, Ginkgo and Gotu Kola to name just a few. GLP receptor agonists and metformin, among pharmaceuticals. i get a feeling that most people here are already doing quite a lot for preserving brain health. The question is for me, what can be done differently from what I (we) do today.
1 Like
The food and supplement angle is surely a minor factor compared to lifestyle effects. A quick search brings up the usual suspects. I’d guess a 1% effect unless the current diet is terrible.
Of course eat a whole food plant based (mostly plants) diet but do as much exercise/ physical activity as possible (ramp up over time) to manifest a more youthful phenotype.
I’m working on an episode with Dr Mike T Nelson that speaks to ways to encourage the body to engage its programming for a more youthful adaptive homeostasis: CO2 tolerance, temperature tolerance, metabolic flexibility, exercise intensity. Push on the extremes to expand the range of tolerable stress. This will encourage the body to adapt into a more physically capable and resilient status …a form of anti-aging, maybe. I’ll find out for myself anyway.
2 Likes
This is the most complete study I have found regarding hypoxia and exercise in relation to periferal vascularization:
TLDR: exercise >hypoxia at least in muscle. Your body adapts to hypoxia, it’s better to focus on the drop in O2.
Based on the study Im going to try a protocol where first you go to hyperoxia and then practice a sprint to induce hypoxia. There is another study in mice where hypoxic sprints didnt provide further improvements in VEGF but I think it’s because the basal level was hypoxic. Let’s see 
Edit: it seems that Lutein/Astaxanthin/Zeaxanthin attenuates the VEGF response from a stressor. This seems to be one of the ways antioxidants blunt adaptations. No way around this but increase the stressor.
2 Likes
Curious
#12
Blood flow restricted training (BFR) show some effects on muscles. But not very much on VEGF.
This is an interesting paper. Thanks
“In regard to skeletal muscle blood flow, capillarization and angio-adaptation, we and others have shown in rodent models and human patients that exercise interventions could represent a powerful therapeutic avenue to prevent, delay or improve alterations in chronic conditions such as peripheral limb ischemia, diabetes, obesity, chronic obstructive pulmonary diseases“
The above statement plus the paper’s wishy-washy “hard to be sure” benefits of low-oxygen availability (chambers, altitude) hypoxia say to me that I should just exercise as much as I can (time, recovery, etc) to get the blood flow and many other benefits of exercise.
This is not to say more benefits cannot be obtained but the investment to payoff ratio and the upside/downside profile worsens the further we go down this rabbit hole.
Nasal breathing during exercise (as well as all other times) can also be helpful in developing a higher tolerance for co2 which improves oxygen delivery to all organs (including the brain), air filtering to protect the lungs, parasympathetic balance for faster recovery and a more stable state of mind, and more.
https://physoc.onlinelibrary.wiley.com/doi/10.1113/EP091571
Peter Attia mentioned this paper in a newsletter, with the following summary:
As expected, the older group demonstrated 32% lower absolute critical power than the young group, but more surprisingly, the disparity persisted after normalizing results for lean mass, with the older group exhibiting 30% lower critical power than the younger group. These findings indicate that losses in muscle mass do not account for most of the difference in critical power between age groups. By examining additional metrics, the investigators concluded that the decline in power was instead related primarily to impaired blood flow and vascular conductance to the working muscles during exercise. Though these data do not establish clear causal links on their own between vascular dysfunction and critical power, the authors propose that reduced blood flow would limit oxygen delivery and waste removal from muscles and might additionally relate to impairments in muscle quality with age.
6 Likes
How can we when we enter later part of life maintain a healthy perfusion of blood in the brain? We know that hypo-perfusion is detrimental (not only in the brain). Exercise is nr 1. Beet juice, small amount of citrulline and other substances might do that trick. What do you think?
The microvascular dysfunction accelerates aging by disrupting tissue oxygen and nutrient delivery, promoting inflammation and oxidative damage, impairing vascular remodeling and repair, and thereby contributing to the decline in organ function and increased susceptibility to age-related diseases. Then there is also the question of what factors is the blood delivering to the cells and how they affect the aging of the cells. Young factors make older organs younger and old factors make young cells older. This video is really fascinating. And I note at the 31 min and 20 sec mark there are data that supports glucosamine being an antiaging supplement to consider.