Sure, it may reduce the risk a bit to get it even lower, but that might come at a cost of higher risk of something else. Personally I don’t like going too extreme on one marker here and don’t think I need to when I got a lot of other things going for me that should lower risk of cardiovascular diseases.
5 Likes
A_User
#632
Lowering to very low levels has very few possible side effects in clinical trials and if there was other ways of reducing progression by proxy of regression with the same level of evidence as the PCSK9 inhibitors in clinical trials I would like to hear about that. I don’t think there exists anything like that.
It will most certainly reduce risk. It will probably stop ASCVD from developing altogether but I don’t know that for sure. The ASCVD process is for sure happening at ApoB 64.
Help, I am confused. “Lipoprotein(a) [Lp(a)] is a cholesteryl ester–rich lipoprotein distinguished from other lipoproteins by the presence of a unique apolipoprotein (apo), apo(a).”
The nomenclature aPoA is not used by my lab nor is ApoA-I. Is it the same as the Lp(a) test?
My own (n-1) experience is that my own Lp(a) level remains relatively constant while my other lipids vary quite a bit. My Lp(a) levels have always been below the Quest Lab threshold while my other lipids are almost always in the normal range. That is why I quit paying for the Lp(a) test.
“Genetic factors play a major role in Lp(a) concentrations. In fact, Lp(a) levels are 70% to 90% genetically determined.”
“A patient’s Lp(a) levels are one of the strongest indicators of their genetic risk for cardiovascular disease,”
https://health.ucdavis.edu/news/headlines/lipoproteina-a-less-understood-but-critical-risk-factor-for-heart-disease/2023/02#:~:text=An%20elevated%20level%20of%20lipoprotein,have%20also%20been%20well%20documented.
1 Like
I found it. My lab uses the term Apolipoprotein A1. The search bar doesn’t recognize the other terms.
2 Likes
cl-user
#635
That’s not Lp(a) which is Lipoprotein (a)
That’s Apolipoprotein A-I (ApoA -I), the major protein component of high density lipoprotein (HDL)
Lp(a) is part of ApoB:
Apolipoprotein B is the primary apolipoprotein of chylomicrons, VLDL, Lp(a), IDL, and LDLparticles
2 Likes
David
#636
This meta-analysis has findings c/w your thoughts. The larger risk reductions are seen in higher baseline levels vs. lower.
I’m not denying the fact that lowering ApoB even when it’s already very low can’t further reduce risk. I just think that in my case the risk reduction will be very small if any at all because my risk is already so low that it might not be significant. As David said, the reductions are larger with higher baseline levels.
I think it’s too much of a generalization when you say “the ASCVD process is for sure happening at ApoB 64”. There are plenty of people with ApoB far higher than that that have no detectable vascular calcification. There are also people with levels much lower than that that have detectible calcification. While ApoB is a very important factor, it’s still just one of many factors. If you have super low ApoB, yet have high levels of inflammation, oxidative stress, high homocysteine, are fat, don’t exercise and etc. then you may still experience a fairly high risk of atherosclerosis. In contrast, if you have low ApoB, yet not super low, you might still have neglegible atherosclerisis if most of the other factors are excellent. Note that people in these studies showing risk reduction from PCSK9 inhibitors are average people and many of those people will have significant risk of atherosclerosis even with a very low ApoB because many other aspects of their health are far from optimized. In contrast, I am in many ways much more healthy than the average person and I don’t think I need to go super low in terms of ApoB to have super low risk. I think it’s better to focus on getting a lot of the most important markers good or very good, than to focus too much on some one best marker and get that one super good.
In addition to this, I avoid taking drugs if possible unless they have a very long history of use and safety. While PSCK9 inhibitors may be pretty safe in the short term, even for many years, we still lack very long term data. I think that’s important for us interested in extreme longevity. In addition, they are expensive and require injections.
Another point. I don’t like focusing too much on ApoB or LDL as the bad causal factor that must be reduced and not taking into account the other side of the coin. Even if your ApoB and LDL are high enough to cause some atherosclerosis, it can be prevented and reversed significantly by reverse cholesterol transport.
7 Likes
Are there any clinical trials done in humans to prove that?
Look up “reverse cholesterol transport”. It’s a well known process that occurs in the body and removes cholesterol from plaque, counteracting cholesterol deposition in the vasculature. HDL cholesterol participates in that process. There are also drugs that have been or are in development that increase reverse cholesterol transport with the goal of reducing or reversing atherosclerosis. One of them is ApoAI Milano. I’m not up to date on these drugs but here is one study as an example: Effect of recombinant ApoA-I Milano on coronary atherosclerosis in patients with acute coronary syndromes: a randomized controlled trial - PubMed
1 Like
Neo
#640
@Olafurpall @A_User
This week is the big American Heart Association congress. So we may see potential interesting updates over the coming days
3 Likes
Didn’t the trials to increase HDL fail to improve outcomes?
Yes, but that’s because the HDL level per se isn’t what’s of most importance here and it isn’t necessarily a good marker of reverse cholesterol transport activity. Instead, it’s the quality (number and size) of the HDL particles which matters more.
3 Likes
A_User
#644
I have another perspective based on building a world model on causal processes.
I am not talking about risk really, I am talking about stopping the causal process from happening altogether.
ApoB/LDL is probably the necessary cause, meaning with very low levels you won’t get heart disease no matter how much you smoke and have bad habits. Genetic studies remove other factors.
I don’t think that includes the mechanism of the causal process, apoB concentration over time, long time.
Here is also a relevant challenge afaik no one has solved:
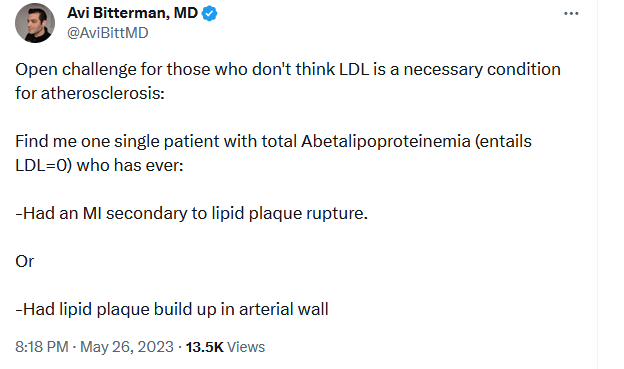

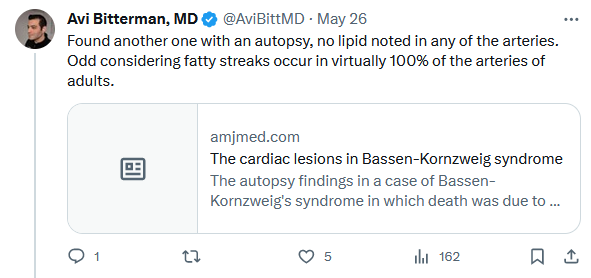
https://twitter.com/AviBittMD/status/1662166874988085250
This, with all the other evidence (rct’s, relationship of ldl and ascvd, genetic studies), suggest to me lipids is the most important factor and can make the other factors irrelevant. I don’t know if you’ve heard of this before. This is quite promising evidence. What are your thoughts?
3 Likes
You notice any lack of muscle development from metformin? I’m thinking about starting it but have seen info claiming metformin inhibits muscle growth?
Thanks
1 Like
I have been taking metformin for decades. It may slow down gains, but I think the effect is small in the long run. The benefits of taking metformin IMO, far outweigh the downsides.
5 Likes
Do you mind sharing your dosage? And any concerns ever about lactic acidosis?
I also do not see an impact on muscle building. I do feel an impact on HIIT training. My mitochondria do not work as efficiently so I make more lactate at lower intensities. I don’t know if that is a bad health thing but it is unpleasant. I take 500mg extended release.
2 Likes
J0hn
#650
I think the lactic acidosis concerns, if my memory serves me correctly was seen with phenformin, which was superseded by metformin.
1 Like