I don’t think this paper has been discussed in the forum before: Dose-Dependent Acute Effects of Everolimus Administration on Immunological, Neuroendocrine and Psychological Parameters in Healthy Men 2020
The rapamycin analogue everolimus (EVR) is a potent inhibitor of the mammalian target of rapamycin (mTOR) and clinically used to prevent allograft rejections as well as tumor growth. The pharmacokinetic and immunosuppressive efficacy of EVR have been extensively reported in patient populations and in vitro studies. However, dose-dependent ex vivo effects upon acute EVR administration in healthy volunteers are rare. Moreover, immunosuppressive drugs are associated with neuroendocrine changes and psychological disturbances. It is largely unknown so far whether and to what extend EVR affects neuroendocrine functions, mood, and anxiety in healthy individuals. Thus, in the present study, we analyzed the effects of three different clinically applied EVR doses (1.5, 2.25, and 3 mg) orally administered 4 times in a 12-hour cycle to healthy male volunteers on immunological, neuroendocrine, and psychological parameters. We observed that oral intake of medium (2.25 mg) and high doses (3 mg) of EVR efficiently suppressed T cell proliferation as well as IL-10 cytokine production in ex vivo mitogen-stimulated peripheral blood mononuclear cell. Further, acute low (1.5 mg) and medium (2.25 mg) EVR administration increased state anxiety levels accompanied by significantly elevated noradrenaline (NA) concentrations. In contrast, high-dose EVR significantly reduced plasma and saliva cortisol as well as NA levels and perceived state anxiety. Hence, these data confirm the acute immunosuppressive effects of the mTOR inhibitor EVR and provide evidence for EVR-induced alterations in neuroendocrine parameters and behavior under physiological conditions in healthy volunteers.
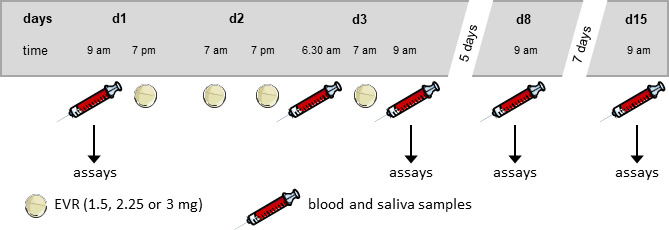
Study design. Three different EVR doses (1.5, 2.25, or 3 mg) were orally administered 4× in a 12-hour cycle to healthy men. Blood and saliva samples were withdrawn before (day (D)1) and after (D3, D8, and D15) oral administration of EVR and subjected to further analysis. EVR, everolimus.
Although impaired mTOR signaling has been implicated in neurocognitive dysfunctions and neurodegenerative processes, it remains uncertain whether and to what extent clinically used doses of the mTOR inhibitor EVR affect neurocognitive and psychological parameters in healthy humans. Our data revealed that an acute EVR administration with low and medium doses induced an increase in state anxiety levels, whereas intake of the high doses did not affect state anxiety. These findings indicate that the induced changes in state anxiety apparently depend on the administered EVR dosage. This notion is supported by studies in rats showing that acute one-time and repeated rapamycin treatment with low doses (1 mg/kg) and high doses (3 mg/kg) resulted in anxiety-related behavior probably induced by mTOR-independent mechanisms leading to hyperexcitability of the amygdala. Moreover, anxiety (e.g., following a drug treatment) has been associated with the perception of drug-induced side effects. The fact that participants hardly reported medication-attributed side effects, although a significant increase of state anxiety was observed in the low-dose and medium-dose groups, indicates that acute intake of therapeutic EVR doses indeed does not induce subjectively perceived side effects.
Anxiety, stress, and depression are directly linked to the activation of the sympathetic nervous system reflected by elevated release of NA and specific brain regions that, in turn, stimulates the HPA axis and the release of cortisol. Because we observed increased NA levels along with not affected cortisol levels after acute EVR intake in the low-dose and medium-dose groups, our data indicate that both EVR doses might lead to an activation of the sympathetic adrenomedullary system probably not accompanied by changes in HPA activity. In contrast, high-dose EVR treatment reduced plasma and saliva cortisol without directly affecting NA level and state anxiety. Whether the reduction in NA levels on D8 and D15 in the high-dose group was directly induced by EVR or rather was mediated by secondary factors (e.g., drug withdrawal (rebound effect)) has to be validated in further experiments. Although plasma NA concentration is a useful parameter to assess sympathetic nerve activity, more functional analyses (i.e., pupillometry, heart rate variability, and/or salivary alpha-amylase activity), might provide more details on the effect of the different EVR doses on sympathetic nerve activity in future research. We observed dose-dependent ex vivo effects of EVR on cytokine production on D3, however, this was not the case for the assessed cortisol and NA levels. These findings indicate specific thresholds for EVR blood concentration that associate with changes in cortisol levels in saliva and plasma as well as NA plasma levels compared with baseline values assessed before drug intake.
The dosing schedule is a bit weird, but do other papers confirm that anxiety increases at low dose but decreases at high dose with everolimus or sirolimus?
Given the half-life, ChatGPT tells me that this dosing schedule is equivalent (in terms of content in the body) to about taking once a 2x larger dose. So 3 mg, 4.5 mg or 6 mg. The equivalence between everolimus and sirolimus is not straightforward but let’s say it’s 1:1.
Then, if the above finding is also true for sirolimus it would mean that one needs higher doses (~6 mg) to avoid sympathetic activation and anxiety?
Could this explain the conflicting reports on the effect of rapa on anxiety, HRV or sleep?
Even more so if you assume that what matters is the mg/kg dose. These healthy young men had BMI ~ 23 kg/m2:
Can this be related to this low-dose risk mentioned here:
@CronosTempi: as you looked at the best starting dose for rapa, what do you think?