tongMD
#1210
I’m not a TCM practitioner but I doubt very many would be offended.
I’d note at the time - they might seem dumb now - but a good amount of these made sense in a way - the classic example - mercury was used for syphilis for lack of antibiotics.
I’d also point out that artemisinin (a derivative of sweet wormwood) for malaria was so huge that Tu Youyou won a Nobel without a PhD or MD degree.
They also used what a version of what we call aspirin (a derivative of willow bark).
1 Like
A_User
#1211
The increase in PCSK9 would lead to increased LDL levels, but the statins already compensated for that?
Also there’s been a study on 40 mg rosuvastatin, there was an increase in lp(a) but it is relatively minor and the decrease risk from overall apoB reduction is higher.
Yes, that sounds like an effective treatment & most bang for the buck for both dose&apoB reduction and apoB reduction&costs. I haven’t heard about weekly dosing. I take 0.83 mg rosuvastatin 3x a week, going to check how apoB moved soon also after stopping berberine. I don’t think I’ll add in ezetimibe unless an increase in rosuvastatin / dosing frequency wouldn’t keep apoB & non-HDL-c at optimal levels. If I had to choose I’d proably take 1 medication over two. Also why I stopped with berberine.
tongMD
#1213
PCSK9 is not just about LDL. There are other functions involved. That’s partly why I have reluctance.
Peter Attia is pro-statins and if you read his articles it’ll seem like he has atherosclerosis all figured out - but that’s not the case. The guy is clearly talented, but note he makes 6 figures per patient practicing VIP medicine and he has a clear incentive to keep it that way - which means doing something that others aren’t. Note he used to be associated with Gary Taubes at Nutrition Science Initaitive which was such a big s***show he quietly disassociated with them. He also very occasionally has a habit of making claims that is completely opposite of the papers he cites or a big stretch (assuming there isn’t human error from his editing team). Few people will notice that because most people do not actually read the research or they are at best skimming the abstract with little to no understanding of the context.
If you read your cited article carefully, he says Lp(a) is not of clinical significance to those where taking statins is indicated. Attia also took statins himself before, but note he stopped more recently. I wonder why as he never really explained it.
I’m not convinced about pleiotropic effects of high-dose statins for “healthy” individuals are of net benefit or if the lowest LDL is the best. I don’t claim to know with as high certainty as Attia seems to point to. I do agree with lowering LDL when it comes to FH. I also do generally agree going on the lower side of apoB is probably worthwhile and I prescribe statins to those who have moderate to high ASCVD risk or multiple risk factors (preferably after a one-time Lp(a) screen if they can afford it out of pocket).
It depends on the statin, but generally, there is a side effect of increased insulin resistance as well that is dose dependent. IR/diabetes is a risk factor for ASCVD risk. Hence, I’m still iffy on low ASCVD risk with one risk-enhancing factor (ie South Asian or autoimmune disease), partly based on ACC 2022 guidelines but as mentioned - I’m going to assume an LDL 70-90 target with lifestyle factors first would be fair. There is some uncertainty for me to jump to statins but I’d be willing to refer to a lipidologist who prescribes say once weekly low-dose 2.5 mg rosuvastatin if a “30-year FRS” is high enough on top of low-dose ezetimibe, assuming everything checks out on minimizing possible adverse effects and pharmacogenetics.
In practice, no insurance is paying for LDL-P/apoB/Lp(a)/solid CLIA-certified WGS testing - at least not in a “healthy” populace right now where I’m at. Pharmacogenetics isn’t an easy topic and I’m surprised Peter Attia actually never really goes in-depth on it for statin side effects.
I don’t know whether LCHF diets (which is what Attia used to strongly push for without enough evidence) would be truly beneficial owing to fewer small LDL particles - my approach to nutrition is going where the evidence subtly points me to directionally, on top of simulating mechanistic effects and my own N-of-1 crossover trials, due to lack of long-term longitudinal studies.
3 Likes
rivasp12
#1214
No one has atherosclerosis figured out. Some may pretend to for various reasons, including monetary, but the subject is just too complex, the evidence keeps evolving and changing, it’s all very conflicting and confusing.
There seems to be little doubt that the cardiac risk factors are additive, and they all need to be carefully considered before starting therapy.
I like some of the natural alternatives like lycopene, Amla, citrus bergamot, and berberine. Very low dose weekly statins may be a good option. Don’t like potential cognitive issues with the statins and a study yesterday demonstrated osteoporosis in mice with high dose statins.
I have no opinion regarding Attia, but I know that he was trained as a surgeon, and my training is in internal medicine. Surgeons and Internists rarely agree on interventions. We tend to be more conservative. Doesn’t make it the right choice.
2 Likes
tongMD
#1215
I’m generally more comfortable with lycopene natural from food (assuming you are very careful how it is produced throughout the supply chain) and I’d be extremely careful about any supplements as anything way more than from diet should be considered a drug in my opinion and supplement quality can be an issue. (Not necessarily a bad thing - but it warrants pharmacovigilance)
As for citrus bergamot supplements, I’d wonder if the coumarins interfere with CYP3A4 to a significant degree, curious as to your experience especially if you tested rapamycin levels in blood.
I’m actually considering adding some citrus peels + cocoa bits + tomatoes (processing actually increases lycopene content btw) though!
2 Likes
Davin8r
#1216
I’ve listened to all of Attia’s podcasts involving lipids and vascular disease. I admire him for his “strong convictions, loosely held” philosophy where his views have evolved over time based on evidence, and he has no problem admitting this. He’s not all-out low carb/high fat in his dietary advice, but rather pragmatic in his approach, i.e. if energy intake restriction is necessary, then a person can do it via intermittent fasting, overall caloric restriction via calorie counting, or macronutrient restriction of fat or carbs (all 3 strategies which have the final common result of reducing energy intake while maintaining high enough protein to help preserve lean mass). He doesn’t claim to have atherosclerosis “all figured out”, but he currently does recommend a lower-is-better approach for ApoB and long-term risk of ASCVD. The Mendelian randomization studies which show such dramatic reductions over life time exposure to low vs high LDL/ApoB have been especially convincing as opposed to what we’re limited to seeing with short term experimental trials (even an expensive trial that lasts 2 years and shows a modest effect of a statin or PCSK9i can’t compare to what would be achievable with keeping ApoB low for 10, 20 or 30+ years). He and Layne Norton go into detail on this topic in this week’s Drive podcast. Of course, we always have to balance lowering LDL pharmacologically with potential side effects. I’m intrigued by the idea of a once weekly low dose statin and might actually give this a try depending on my blood work results next week.
3 Likes
tongMD
#1217
Gary Taubes is still on Peter Attia’s podcast btw. The funny thing is if you look at the 501c3 salary - Taubes salary seems to be more reasonable than Attia.
It’s not completely damning, nor am I claiming “Attia is a horrible person”, but it should be more than enough to hold some pause when Attia makes strong claims with certain incentives. Not to mention, still has Mark Hyman and Jason Fung on his podcast - despite the Nutrition Science crusade debacle.
I’m not pro-statin or anti-statins. I prefer to read the research directly with as much context as possible, rather than go on “guru” claims - especially when others on his podcast have been heavily debunked.
https://sciencebasedmedicine.org/tag/mark-hyman/
1 Like
rivasp12
#1218
Here’s an interesting theoretical question posed by a Dr.on Twitter
Davin8r
#1219
I’d answer that with my own theoretical question: “So those 70 year old smokers who don’t have lung cancer or COPD should have quit smoking when they were 30? Show me the evidence.”
Selection bias. Again, I see ApoB particles as necessary but not sufficient for ASCVD, and I agree that there are mitigating factors such as inflammation, oxidative stress, etc. Attia even made an offhand comment on a recent podcast, to the effect of “some people just seem to be immune” to ASCVD despite their lipids, blood pressure and lifestyle factors.
Until we find out the mechanisms of that protection and how how to safely and reliably replicate it in humans, ApoB is a great target IMO.
4 Likes
rivasp12
#1220
Haha
Clever answer with the smokers analogy.
1 Like
Davin8r
#1221
Thanks!  I admit it’s not a perfect analogy, since all life-long smokers will presumably have tar in their lungs, whereas not all of those with high ApoB will have coronary calcification.
I admit it’s not a perfect analogy, since all life-long smokers will presumably have tar in their lungs, whereas not all of those with high ApoB will have coronary calcification.
I haven’t looked into this, but I wonder if there’s such a thing as a phenotype where there are multiple/numerous soft atherosclerotic plaques in the vasculature but very little calcified plaques, and if this phenotype can persist over time without accruing calcified plaques while at the same time being at significant risk of ASCVD events(?)
I did a page looking at Gene Expression/Acetyl-CoA/Long Gene issues which has some links on ASCVD that people might find interesting.
tongMD
#1223
There are a lot of wrenches here - the most obvious being the paradox in much higher CAC scores and statin usage.
Statins can calcify plaque and increase CAC - appears to be more stable - difficult to tell whether you can use CAC as a prognostic indicator unless you are drug naive.
“Statin therapy modestly accelerates calcification of plaques leading to more stable, lower-risk compositions and sometimes an acceleration of Agatston CAC score progression. The prognostic utility of CAC in statin users is not well characterized.”
1 Like
This clip is from podcast # 235
Interesting discussion with Peter Atia with Layne Norton, Ph.D. especially the independent risk factor of LDL.
@ 5:44 Layne Norton: “We still have LDL denialists out there”, Peter Attia: “I think it is one of the most dangerous things I see actually.”
1 Like
rivasp12
#1225
That’s an overly simplistic view and ignores the evidence of multiple studies as being essentially irrelevant.
1 Like
rivasp12
#1226
Here’s a new 10 year study just published looking at lipids and CVD. It emphasizes the complex nature of this topic and it’s anything but settled and simple.
“ However, evidence supporting the causal link between TC, LDL and CVD remains controversial, and recent data reveals that CVD risk cannot be merely explained by TC and LDL levels, that LDL might even be Beneficial in terms of overall lifespan and that treatment with statins is of doubtful benefit in regard to primary CVD prevention.”
In this study HDL and Triglycerides were found to be the highest predictors, but it varied significantly by subtype.
The lipid/ CVD story is complicated and is still being written. Anyone suggesting otherwise is being overly simplistic.
1 Like
A_User
#1227
Because they are lower in the evidence hiearchy. Don’t you use this heuristic too? Life is too short to be considering all the evidence, especially the weaker types (lower on the hierarchy).
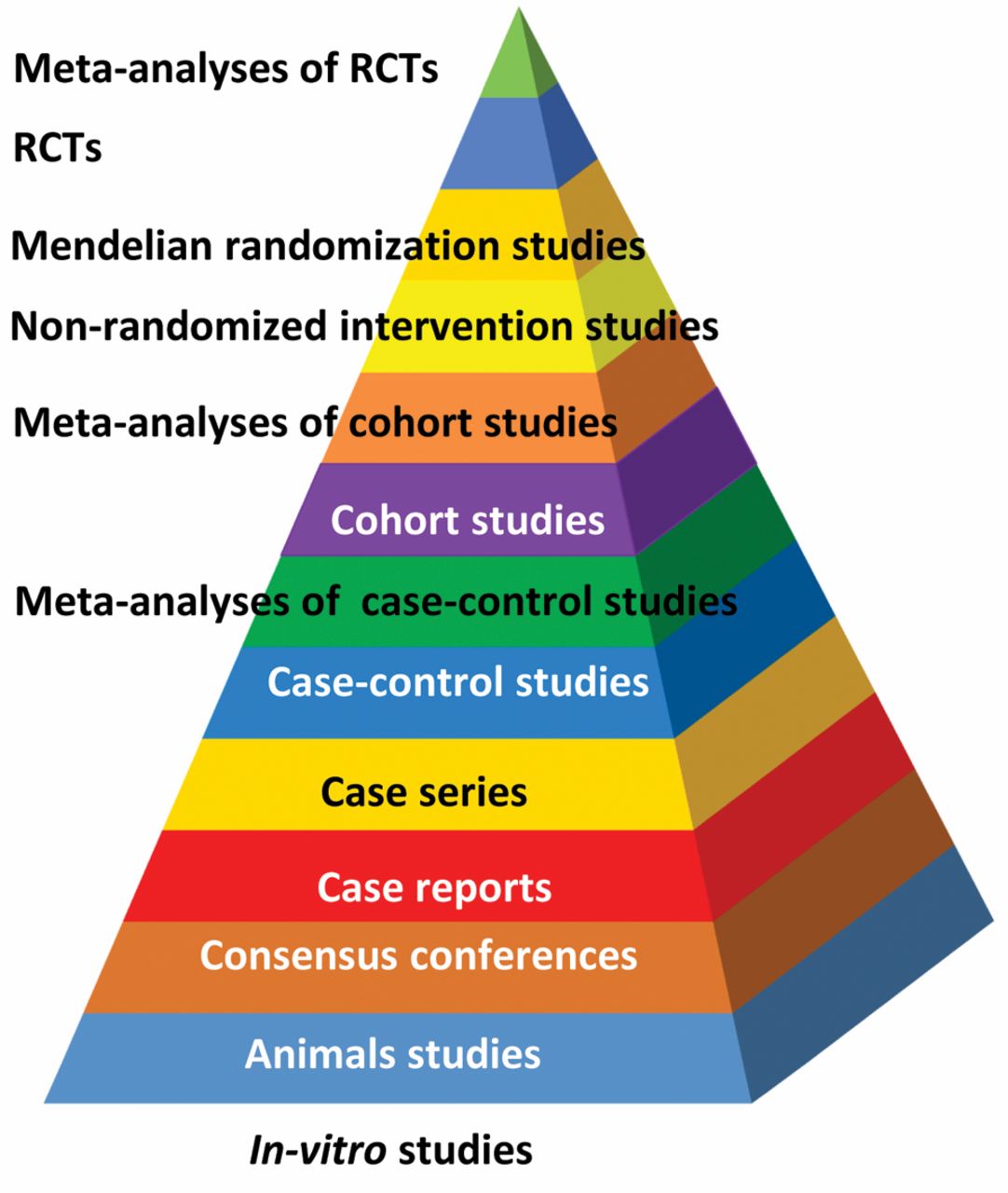
3 Likes
rivasp12
#1228
Actually, for many people, life is too short for them to have an open mind and consider thoughtfully any study that conflicts with their pre- established viewpoint.
Life is complicated and paradoxical.
4 Likes
Arhu
#1229
So finally we know why rapamycin moves some markers in the wrong direction, it’s because it’s actually doing its job and autophagy is kicking in
2 Likes
In essence one of the issues with markers. Sometimes you can only make progress by having the side effect of one or more markers going the wrong way. A strong argument for cycling really.