Yes, I think the pandemic really disrupted depression data everywhere, so I usually deprecate that period. But ok, I take your word for it, that you didn’t notice any regional differences. Maybe because I’m in France usually just once a year for the film festival, I tend to notice differences I wouldn’t perceive if living there constantly (I lived in Paris for a couple of years in the 80’s, though, ancient times probably before you were born, a different world!). I fly into Paris, stay for a few days, then fly to Nice and go to Cannes. That’s how I compare Paris people to the people around Cannes, but of course could be my subjective wrong impression. Clearly you have a different impression.
1 Like
medaura
#619
DHA can play important roles in brain physiology without necessarily increasing the volume of the hippocampus or of any other brain region. It could be essential as a building block of normal sized and normal functioning brain regions. The much increased demands during pregnancy seem to suggest as much. Proteins get cycled over for all cells all the time. Fat membranes probably do too so you need the building blocks in adequate supply.
Even rapamycin increasing hippocampal volume doesn’t seem like necessarily a gift with no strings attached as, from what I read, comes with synaptic density loss.
Again for cognition, it doesn’t need to act as a nootropic to support cognition. It might just be the type of oil to keep the engine running instead of giving you an engine upgrade — as the increased hippocampal volume might be considered analogous to.
What you said was that the study proved DHA to be useless for cognition when it shows no such thing, with all the signals pointing in the opposite direction. Earlier in the thread you said it doesn’t even penetrate the brains of apoE4 carriers based on mice data. But the study in humans showed that indeed it does. So that’s not a problem either.
It is very interesting how exogenous supplementation seems to down regulate endogenous supply but there’s many ways to look at that. One obvious possible interpretation is that DHA is so important to the body that in the absence of exogenous supply the body will make some of its own. That doesn’t mean it will make it at rates optimal for longevity or cognition. I’m sure the body follows its own economics in allocating scarce resources. The synthesis might be costly so it stops once adequate outside supplementation is secured.
Plasmalogen supply has this self regulating feedback loop too, with exogenous supply limiting endogenous synthesis. That doesn’t mean supplementing with them is useless. I feel the effects of supplementation pretty clearly first hand.
It can also be that at some point in later life for apoE4 carriers the negative feedback loop turns into a positive feedback loop, with chronic absence of DHA leading to the breakdown of machinery that would synthesize it internally or be responsible for its transport past the BBB so the poor get poorer and, as data shows, DHA supplementation being useless at increasing brain levels of DHA once Alzheimer’s has kicked in.
At any rate this is speculative and complicated but your conclusion that DHA is useless for cognition especially for apoE4 carriers doesn’t seem warranted.
1 Like
adssx
#620
RCT and MR found nothing (see: Vitamin O (Omega 3) for athletes - #4 by adssx ).
If it was about a long exposure before dementia onset, then surely this should be captured by MR studies?
Do vegans live shorter or have more AD? Did DHA supplementation increase mice lifespan in the ITP?
So: what is the evidence in favor of DHA supplementation? Association studies (even those favor EPA)? Or some mechanistic hypothesis? That’s quite weak.
2 Likes
Paper:
Potential benefits of kefir and its compounds on Alzheimer’s disease: A systematic review
This systematic review, conducted in January 2024, examined the effects of kefir in both in vivo animal models and human patients with neurodegenerative conditions. The review was based on studies retrieved from BVS, Embase, PubMed/MEDLINE, Scopus, and Web of Science databases. Seven studies were included, involving invertebrates, murine models, and human participants. In animal models, the primary outcomes were antioxidant effects, reduced beta-amyloid deposition, and attenuation of vascular damage and neurodegeneration. In human studies, kefir supplementation resulted in decreased levels of inflammatory cytokines, reactive oxygen species (ROS), and oxidative proteins, and was associated with improvements in memory. Given its potential benefits, kefir could serve as a valuable adjunct to conventional treatments for Alzheimer’s disease, warranting further investigation in clinical settings.
Paywalled review paper:
https://www.sciencedirect.com/science/article/pii/S2949834125000133
2 Likes
adssx
#622
Regarding fish, this paper (Omega-3 and Risk of atrial fibrillation: Vagally-mediated double-edged sword) concludes that “Higher consumption of dietary omega-3 is associated with decreased AF risk. In contrast, pharmaceutical dosing of omega-3 increases AF in a dose-dependent manner, which may be mediated by vagal tone.”
The RCTs reported that treatment with DHA and/or EPA was associated with a 24 % increased relative risk of AF (absolute risk 4.0 % vs 3.3 %; relative risk [RR] 1.24, 95 % confidence interval [CI] 1.11–1.38, p = 0.0002). This was dose-dependent; DHA + EPA doses of ∼1000 mg/d increased AF risk ∼12 %, whereas 1800 to 4000 mg/d increased AF risk by ∼50 %. In contrast, observational studies focused on DHA + EPA blood levels or dietary intake have generally reported that higher omega-3 levels/consumption are associated with lower AF risk. Maximal AF risk reduction. (12 %) occurred at ∼650 mg/d of dietary DHA + EPA. Other studies have indicated that omega-3 fatty acids can dose-dependently increase vagal tone, which could explain the biphasic relationship between DHA + EPA and AF risk. Experimental studies show that low-level vagal stimulation decreases risk of AF, whereas high-level vagal stimulation increases risk of AF.
So, yes, @Neo: eating fish is good, while supplementation might be risky. (Paper by Bill Harris btw @约瑟夫_拉维尔.)
2 Likes
Neo
#623
Btw - as we just looked at a lot of MR omega 3 data, I thought I’d share the below with people to help out those in context in this specific case:
I quickly discussed whether MR instruments for omega 3 are good with 4o, and this seems like a case where the instruments are not that good and hence MR may not be that valuable, for example outputs from 4o:
Several genome-wide association studies (GWAS), such as those from the UK Biobank and CHARGE consortium, have identified SNPs associated with plasma or red blood cell levels of EPA and DHA. However, these SNPs typically explain only a small proportion of variance in fatty acid levels (e.g., ~1-5%).
Pleiotropy Risk: Variants in FADS1/FADS2 influence both omega-3 and omega-6 pathways, complicating causal inference.
In cases where the instruments are great (clear, explain large portion of the variance) MR analysis can be the most amazing sets of evidence. Here it may bot be the case that instruments are reliable though.
And especially not for DHA
Instruments tend to be stronger for EPA than for DHA, likely due to more consistent GWAS associations.
Btw - I haven’t looked at the studies, but does seem like the inflammation benefits still is picked up:
Some MR studies show modest protective associations with inflammation markers (e.g., CRP), but these need replication.
Her is 4o’s conclusion
Mendelian randomization instruments for EPA and DHA are valid but modest in strength, especially compared to other traits like LDL or BMI. They’re useful for triangulating evidence, but limited power and pleiotropy must be carefully considered. For targeted questions (e.g., DHA and cognitive aging), stronger instruments or well-powered GWAS may still be needed.
2 Likes
Neo
#624
For those in US
not sure if it’s temporary or not, but goodrx has
big discount on this right now (more than 3/4ths off)
https://www.goodrx.com/vascepa?label_override=vascepa&form=capsule&dosage=1g&quantity=120&drugId=36935
3 Likes
cl-user
#625
I agree with you. MR studies are only as good as the proxies they use.
The other issue are the confounders which can be very strong especially for something like EPA/DHA which are very popular supplements as well as found in the diet.
Weak instruments and strong confounders will produce meaningless outcomes.
1 Like
Alzheimer Prevention Talks: A Conversation with an Alzheimer’s Expert
Virtual Event: Wednesday, Apr. 16 7:00–7:30pm ET / 4:00–4:30pm PT
Don’t miss the inaugural Alzheimer Prevention Talks: APT Webstudy Webinar featuring world-renowned Alzheimer’s expert and Alzheimer’s Therapeutic Research Institute Director, Dr. Paul Aisen, in conversation with a clinical trial participant spokesperson discussing the latest changes to the APT Webstudy, updates on the state of Alzheimer’s research, and much more. This webinar series is designed to keep APT Webstudy participants informed about how their participation is advancing the field of Alzheimer’s research.
If you have any friends or family that may be interested in learning about the importance of participation in Alzheimer’s research, please feel free to share this invitation with them.
What:
- Updates on the APT Webstudy, including current progress and upcoming changes affecting participation;
- Why your ongoing participation is vital;
- Other new developments in Alzheimer’s research that are of interest; and more.
Who:
-
Guest Presenter: Dr. Paul Aisen—Alzheimer’s Therapeutic Research Institute; Director
-
Guest Host: Lupe Morales—APT Webstudy; Co-Chair of the ACTC Research Partnership Alliance
When:
Wednesday, Apr. 16, 2025
7:00–7:30pm ET / 4:00–4:30pm PT
Register here
3 Likes
While this all may be true about MRs, when the RCTs are also in the same direction (negative), hard to ignore the preponderance of evidence here.
1 Like
adssx
#628
Thanks. Really good point. I asked to ChatGPT 4.5: ChatGPT - MR Studies on EPA DHA
Most interesting bit:
- Direction of bias
When SNPs explain little variance, there’s a greater risk of Type II error (missing a real effect), not Type I (finding a false effect). So if a strong signal does appear despite low variance explained, it’s often more impressive — though still needs caution.
And the conclusion:
Yes — a significant MR finding can be strong even with SNPs that explain only a small fraction of variance, but only if the instruments are valid and the assumptions are met. In fact, finding significance despite limited variance can indicate a real and potentially important biological effect. Still, MR is best interpreted as part of a triangulation approach with RCTs, biology, and observational data.
So when MR studies find that DHA is a risk factor for colorectal cancer, lung cancer and cardiovascular disease while EPA is protective against depression, coronary heart disease and myocardial infarction: these are HUGE findings, as they were found despite a low variance.
On the other hand, for MR that find no associations (for examples EPA and DHA with dementia) one has to look at the details (F-statistics, effect size, confidence intervals, consistency across methods, etc.) and whether this aligns with RCTs. That’s the case.
2 Likes
cl-user
#629
Sure, and I must admit that @adssx arguments against DHA look more and more convincing.
I was just making a point about MR in general because a lot of people think they are even better than RCTs while they are clearly not. It’s just another tool with its pro and cons like RCTs, epidemiological studies, etc.
There is a specific issue with MR though. Any grad student (anybody even) can use the MR tools and generate a “study” about anything in a few hours and at no cost. Most of them are meaningless and should be ignored but it takes time and effort to rule them out.
That said there are also truly insightful MR studies. It’s just that being an MR study should not be perceived as the highest level of evidence. Same for RCTs and the rest obviously.
2 Likes
Neo
#630
That’s helpful re variance being small.
—
There was another big type of issue with Omega 3 MR instruments though:
Pleiotropy Risk : Variants in FADS1/FADS2 influence both omega-3 and omega-6 pathways, complicating causal inference.
What are your and your AIs thoughts on that?
1 Like
Neo
#631
I do think you want to throw out the baby with the bathwater
For something things where the instruments are clean, clear and explain a lot of the variance they can be hugely important and perhaps more valuable or as valuable as short term RCT in sick people only when you are trying to understand the long term effect and in a population that is healthy or not like that specific clinical trial.
1 Like
adssx
#632
My thoughts: I don’t know enough.
ChatGPT 4.5: ChatGPT - MR Studies on EPA DHA
tl;dr: “Cautious conclusions: The presence of pleiotropy means MR results based solely on FADS variants require careful interpretation and additional verification (e.g., using sensitivity methods or other SNPs).”
So did the MR only used FADS variants or other variants as well? I don’t know, for instance this paper does not even mention “FADS”: Medicine
1 Like
adssx
#633
Unfortunately, the more I dig, the more I’m convinced that DHA is detrimental. I emailed or tweeted my questions to Yassine Hussein (PI behind PreventE4, here), Matt Kaerberlein, Brad Stanfield, Kellyann Niotis, Thomas Dayspring, Rhonda Patrick, and OmegaQuant. Let’s see if one of them gets back to me… Hopefully, someone will prove me wrong but so far it doesn’t look really good for DHA supplementation…
6 Likes
A_User
#635
This looks like horizontal pleiotropy according to this paper (SNP’s can affect Omega-3 and Omega-6 to a specific outcome, or maybe one SNP to two factors before the outcome), here it’s education, intelligence, and schizophrenia:
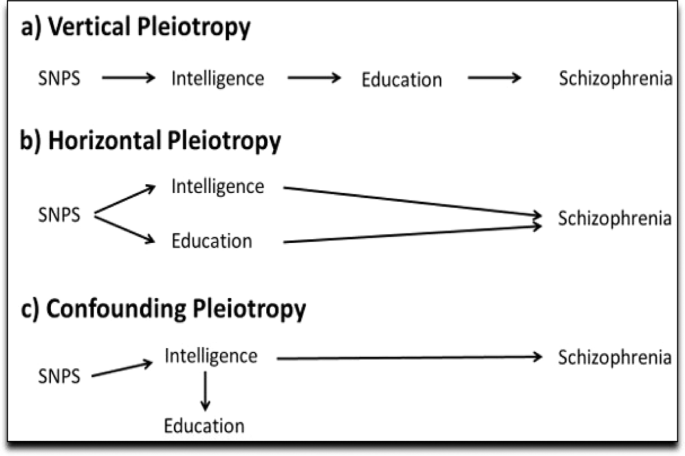
So would need to in that case do Multivariable MR on a possible confounding factor and account for it (in this case Omega-6 if it seems relevant). Is this correct do you think? If so you would check (1) what factor you believe is relevant in horizontal pleiotropy (2) if the study authors did a multivariable MR analysis with that factor, if not, why.
A multivariable Mendelian randomization to appraise the pleiotropy between intelligence, education, and bipolar disorder in relation to schizophrenia 2020
2 Likes
A_User
#636
Although we only used 1–3 SNPs as instrumental variables for each PUFA, the SNPs explained a relatively large variation in PUFA levels and they fulfilled the criterion as not being weak instrumental variables (F statistic > 10)
Study: Polyunsaturated fatty acids and risk of Alzheimer’s disease: a Mendelian randomization study 2019
Regarding instrument relevance, we have selected independent SNPs strongly associated with circulating PUFA concentration, which explained from 4.8 to 7.9% of phenotypic variance (mean F statistics 109–201) among the UK Biobank participants (discovery sample). In addition, we replicated these associations in an independent dataset [12] using the same NMR metabolomics platform as the one used in the UK Biobank participants (median sample size 13,516), where SNPs explained 3.1 to 6.9% of phenotypic variance in circulating PUFA. This indicates that bias due to weak instruments is unlikely to be substantial in our analyses, even though bias due to winner’s curse (due to using the UK Biobank to select SNPs and estimate their effect on PUFA) could affect the magnitude of effect estimates.
Study: Role of circulating polyunsaturated fatty acids on cardiovascular diseases risk: analysis using Mendelian randomization and fatty acid genetic association data from over 114,000 UK Biobank participants 2022
Mean F-statistics were 120- 8572 for UKBB fatty acid exposures and 15–6315 for FADS analyses, suggesting these analyses were unlikely to be substantially biased by weak instruments (Table S4). Mean F statistics for EPA analyses were 9, leading to possible weak instrument bias.
Study: Omega-3 fatty acids and major depression: a Mendelian randomization study 2024
–
I checked three MR papers and they seemed good with regards to weak instruments based on what they said.
Do people even publicize if they don’t have a good F-statistic (statistical power)/weak instrument? Might not pass peer review?
As a general rule, an F-statistic >10 indicates that the level of weak instrument bias is likely to be small. F-statistics should not be used to select IVs to avoid overfitting the estimation model. For example, an F-statistic of <10 does not indicate that an IV should not be used but, instead, it should be noted in the analysis that weak instrument bias should be a considered limitation.
https://mr-dictionary.mrcieu.ac.uk/term/f-statistic/
1 Like
Dr.Bart
#637
add Nicolas Verhoeven, PhD - Physionic - he’s a pure science guy, he doesn’t preach just dissects studies
2 Likes