LaraPo
#29
How islet cells necrosis would manifest itself? Would it contribute to pancreatic cysts? I did develop a few pancreatic cysts, very small. I suspect Rapa bc I’m on it for 14 years. I take 0.5mg for 4-5 days and break for 5 days. This is the smallest dose I have ever had.
2 Likes
That is interesting, but its in a group that is already diabetic. What we really need to look at are non-diabetic populations I would think.
I found this interesting:
Our data suggest that many changes in islet structure and function associated with diabetes are attributable to hyperglycaemia alone and are reversed when blood glucose is normalized.
from:
Reversible changes in pancreatic islet structure and function produced by elevated blood glucose
https://www.nature.com/articles/ncomms5639
4 Likes
Sure, but the untreated diabetic group still had healthier islets than the diabetic group treated with rapamycin.
4 Likes
Here are some pathways that lead to islet cell necrosis.
Via https://www.researchgate.net/figure/Mechanisms-of-islet-cell-death-Flow-chart-depicts-apoptotic-and-necrotic-beta-cell-death_fig2_6336327
Caption: Mechanisms of islet cell death. Flow chart depicts apoptotic and necrotic beta cell death cascades along with possible modes of intervention. Causes/agents of beta cell death are indicated in red while agents/strategies for prevention of beta cell damage are indicated in blue. Red arrows stand for possible sites of intervention.
4 Likes
Shady
#33
Evidence of Rapamycin Toxicity in Pancreatic B-Cells and a Review of the Underlying Molecular Mechanisms. Barlow, et al. 2013.
Roles of mTOR in the Regulation of Pancreatic β-Cell Mass and Insulin Secretion. Asahara, et al. 2022.
The top paper is what peaked my interest in this topic. Also the fact that Rapamycin induced DM is only partially reversible by discontinuation (lab animals) leads me to believe this is something more than physiologic insulin resistance that occurs in a starvation scenario. The latter is completely resolved, not partially, by restoring energy balance in the subject.
5 Likes
Neo
#34
What are people’s thoughts?
Yes, given how important glucose regulation and overall metabolic health is for longevity it seems crucial to gain as much understanding here as we can.
Do the potential permanent changes to pancreatic function due to rapa occur from current “longevity dosing” or only from “transplant level dosing”?
Both papers are linked below and with abstract. It does seems like the first one and more recent ones of that nature are key to understand.
@Krister_Kauppi can you ask your various rapa experts about this and you interview them?
2013 Review
Evidence for rapamycin toxicity in pancreatic β-cells and a review of the underlying molecular mechanisms
Rapamycin is used frequently in both transplantation and oncology. Although historically thought to have little diabetogenic effect, there is growing evidence of β-cell toxicity. This Review draws evidence for rapamycin toxicity from clinical studies of islet and renal transplantation, and of rapamycin as an anticancer agent, as well as from experimental studies. Together, these studies provide evidence that rapamycin has significant detrimental effects on β-cell function and survival and peripheral insulin resistance. The mechanism of action of rapamycin is via inhibition of mammalian target of rapamycin (mTOR). This Review describes the complex mTOR signaling pathways, which control vital cellular functions including mRNA translation, cell proliferation, cell growth, differentiation, angiogenesis, and apoptosis, and examines molecular mechanisms for rapamycin toxicity in β-cells. These mechanisms include reductions in β-cell size, mass, proliferation and insulin secretion alongside increases in apoptosis, autophagy, and peripheral insulin resistance. These data bring into question the use of rapamycin as an immunosuppressant in islet transplantation and as a second-line agent in other transplant recipients developing new-onset diabetes after transplantation with calcineurin inhibitors. It also highlights the importance of close monitoring of blood glucose levels in patients taking rapamycin as an anticancer treatment, particularly those with preexisting glucose intolerance.
2022
Roles of mTOR in the Regulation of Pancreatic β-Cell Mass and Insulin Secretion
Pancreatic β-cells are the only type of cells that can control glycemic levels via insulin secretion. Thus, to explore the mechanisms underlying pancreatic β-cell failure, many reports have clarified the roles of important molecules, such as the mechanistic target of rapamycin (mTOR), which is a central regulator of metabolic and nutrient cues. Studies have uncovered the roles of mTOR in the function of β-cells and the progression of diabetes, and they suggest that mTOR has both positive and negative effects on pancreatic β-cells in the development of diabetes.
At the same time, however, it remains controversial whether mTOR provides a benefit or a risk to pancreatic β-cells [29]. Therefore, in this review, we introduce reports on the role of mTOR in pancreatic β-cells and focus on the positive and negative effects of mTOR on them.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9138643/
8 Likes
For today’s update, my fasting glucose overnight and before my first meal went from 80-95 pre-rapamycin to 95-110 post-rapamycin @ 2mg taken 24 hours ago.
It no longer goes down to the mid 90s 6-7 hours after a meal but stays at 100-110.
Edit- I’ve noticed my gums are a very healthy pink. I noticed this morning when I brushed my teeth and again tonight. I don’t have gingivitis or any dental issues but my gums were a bit darker pink than it is now. Could be nothing but I’m aware of the oral health study happening at UW, and it’d make sense that rapa would lower gum inflammation.
For what it might be worth, this is my 8th day on rapamycin 1mg per week, so my second dose today. Started with a CGM in Jan, then daily X 4 months. I was surprised with excursions of my BS to 200 mg/dl range after a “normal meal” despite an A1c of ~5.7. So changed my diet abruptly to no added sugars and lots of fats/protein (so bacon & eggs, half-n-half, heavy cream, lots of nuts, lots of meat at dinner). I fast ~16 hrs/day but for many years.
Re: exercise, some might call my exercise regimen as “heavy exercise” but it’s been my daily regimen for years- 9000 steps on the backside of the local dam with 4500 up, 4500 down steps with no flat spots, no rest, then 50 pushups. I’m 72 yrs old, 6’2" 180 lbs.
Upon awakening, BS immediately rises about 10 points (probably in anticipation of my morning stairs) from maybe 97 to 107, and then during “my stairs”, it might drop to high 80’s, but then immediately pops up about 10 pts on completion of my stairs. I’ve not been on a CGM since started rapamycin but will break one out and monitor. I have been using a glucometer about 5x daily though and surprised that rapamycin has not appeared to raise my BS’s (but a CGM will more accurate).
Will update later with CGM data now that I am on rapamycin.
7 Likes
Freestyle Libre sensors are known to be inaccurate and you can’t calibrate them like you can with Dexcom sensors.
GregE
#38
Dr. Green’s Rapamycintherapy.com practice has consistently recommended Rapamycin combined with metformin…for me its been 500mg Metformin ER twice daily. I think Nir Barzili’s research and all testing combining R with acarabose/metformin spike longeivty results from 28% to 34%.
Age 70, male, on R and Metformin since 9/2017.
Best of luck to you!
2 Likes
Very interesting! I think this can be a question I dive into together with David Sabatini and Dudley Lamming. I think these two may give the best answer to the question. Let me know if you have any other people in mind because I think it may be to deep for other guests.
5 Likes
Update 24hrs after my rapamycin 1mg dose yesterday. I broke out a Dexcom G7 CGM and applied it. When I wore a CGM x 4 months, I captured the data and put it into SQL Server (a powerful database system) so that I could do queries (such as what is my average glucose from 1:00 pm to 4:00 pm; stuff like that). My G7 read 108 & my glucometer read 107, so it’s well calibrated. My BS, after 24 hrs seems to be running 8 mg/dl higher with rapamycin but I will need to monitor for longer.
I am on 1000mg metformin each evening and have been since I learned of my BS excursions.
My CGM showed this saw-tooth pattern last evening after eating with my blood sugar spiking up and then down, then up, then down, X 4 of these up/down patterns over 3 hrs. That is a new pattern. I will monitor.
Last Tues and then today (the day after 1mg dose) I had a very strong defecation reflex while exercising, so urgent that I had to return home early last week and then this morning, I had to resort to the porta-potty nearby. (Not to be too graphic, but I can see why homeless prefer the sidewalk over a porta-potty). I will monitor this possible side effect too (Do I have a choice?).
I am still getting daily runs of PVC’s, usually trigeminy, but tolerable and waxing and waning over maybe 30 min.
4 Likes
My CGM showed this saw-tooth pattern last evening after eating with my blood sugar spiking up and then down, then up, then down, X 4 of these up/down patterns over 3 hrs. That is a new pattern. I will monitor.
That’s fascinating - that’s what I saw the first day I took my dose too and what prompted me to start this thread.
The first spike was my meal. The red vertical line is when I first took 2mg and in the hours after my glucose spiked up and down multiple times before settling at a level ~10 mg/dl higher than usual similar to you.
Last night at ~1 AM (84 hours after the dose), my fasting glucose levels went back down to pre-rapamycin levels. I woke up in the 80s today which hadn’t happened since I started. I’m guessing the concentration in my blood has dropped to a level where it’s no longer affecting my pancreatic beta cells.
2 Likes
Fantastic, thats the sort of effort needed to really parse out what is happening here.
That saw tooth pattern is very unusual, can’t say I’ve ever seen anything like that.
This is what my CGM typically shows (when I’m taking an SGLT2 inhibitor) - and its usually under-representing the real blood sugar measures (via finger prick) by 10 to 20 points:
Neo
#43
That’s great. Are there any of them that also are more medically trained and/or have spent time on diabetes in their career - that might help as they’ll understand the beta cell biology
Perhaps also ask Matt K? He seems to really want to understand things relation to rapa and might go deep to really figure it out if he had not looked at it before.
1 Like
Both Lamming and Sabatini has looked at the risk of glucose dysregulation so I think they are good. Maybe Peter Attia would be great to ask when I have in on. Matt is great but it will take a time before I have him on again because there are so many other guests that I need to interview  But send that question as a proposal to the Optispan podcast because they are working on some upcoming AMA:s around Rapamycin.
But send that question as a proposal to the Optispan podcast because they are working on some upcoming AMA:s around Rapamycin.
3 Likes
PBJ
#45
From what I see so far, even more reason to fast for a day after taking Rapa.
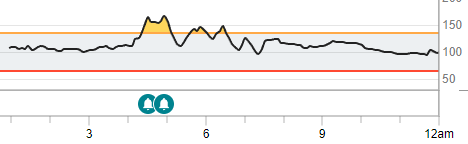
Here is mine from last evening. “Breakfast burrito” for dinner (scrambled eggs/bacon/gruyere cheese rolled up in a tortilla- the tortilla was a mistake!). But my exercise pattern requires lots of calories.
1 Like
I am a Type 2 Diabetic and I was working my way up to the 6 mg dose/week and once I got to 4 mg/week I found that my blood sugar really went up. It had been going up steadily on 1,2 & 3 mg but 4 really made a difference I take Farxiga, Metformin 500mg twice/day and Ozempic. I do not want my Dr. to put me on insulin so I stopped my dose at 3 mg/week. I know it’s not what is recommended for longevity but I am hoping that taking some amount of the rapamycin will help some. If my A1C comes back way high I may have t cut it back still more. We shall see with my next blood test. I do wear a CGM constantly also.
2 Likes
Hi and welcome to the site.
I would be hesitant to use rapamycin if I had diabetes and showed any signs of blood glucose disregulation.
In one of the few studies in mice where rapamycin actually reduced lifespan, it was in the diabetic mouse model.
Adjusting for gender differences, rapamycin increased the mortality risk 1.7-fold in both male and female db/db mice. End-of-life pathological data showed that suppurative inflammation was the main cause of death in the db/db mice, which is enhanced slightly by rapamycin treatment.
全文: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4906320/
3 Likes