cl-user
#162
Here it is. This one is particularly interesting because it has CVD and all cause mortalities.
It is consistent with all the similar studies:
- High TC is only bad below 60 and good after 60.
- High APOB is bad below 60 and don’t care after 60.
- Very high APOB is very bad below 60 and slightly bad after 60.
- Very low TC and APOB are always bad or trending bad.
- High TG is always bad.
- Low APOA1 (HDL) is always bad.
From
The association of apolipoproteins with later‐life all‐cause and cardiovascular mortality: a population‐based study stratified by age
4 Likes
However if we expect to have longer lifespans than regular folks, we may want to keep ApoB and TG lower for longer.
4 Likes
cl-user
#164
it’s not what the plots show.
Very low TC is always bad for all cause mortality for all age groups.
Very low TC is trending bad for CVD mortality for all age groups though not statistically significant.
So if you have a too low TC you die sooner.
For APOB there is no significant effect for very low, low or medium levels.
Very low APOB is trending bad though not statistically significant.
High and very high APOB is bad.
So keep your APOB low of medium. Extremes are bad.
In all cases TG is bad and low HDL (APOA1) is bad.
L_H
#165
I think we can only say that very low TC is associated with por all cause mortality. It may or may not be bad.
3 Likes
cl-user
#166
Yes, that’s correct! These do not imply causality.
3 Likes
Sorry, I made a typo. I meant TG not TC. I agree with both of you.
LaraPo
#168
Actually your debates with youthful assertiveness ( ) were pretty educational for me. I learnt a lot. So, keep debating!
) were pretty educational for me. I learnt a lot. So, keep debating!
3 Likes
adssx
#169
Thanks.
But people with low ApoB probably have low TC as well?
Could it be that you want to minimize ApoB while maximizing some “good” cholesterol (that is probably more complex than just “HDL”).
As I said earlier what I’d love to see is a two dimensional chart with ApoB and TC (or HDL or some HDL subtypes as it seems that quality matter).
Could be done in 3D like this:
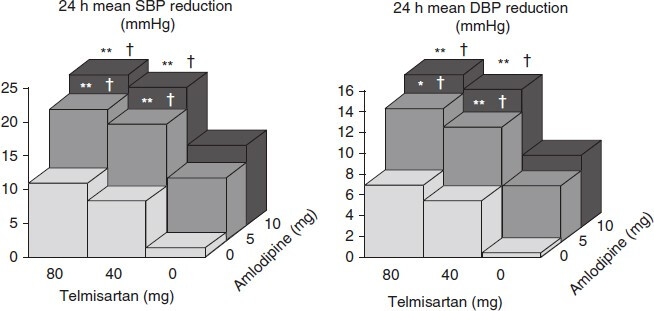
3 Likes
scta123
#170
I believe that what matters most is the process of reverse cholesterol transport. It’s not just about the composition of HDL-C or quantity of apoA-1 particles, but rather the effectiveness of removing cholesterol from tissues. Unfortunately, this process cannot be easily measured and is not fully understood yet. Once we find a medical intervention to address this issue, then we can consider the end of ASCVD IMO.
3 Likes
adssx
#171
What makes you believe this?
2 Likes
Neo
#172
1 Like
adssx
#173
2016 paper with 0 recent citations: is there more recent progress in this field? (I don’t know anything about this topic)
1 Like
While researching CETP inhibition, I came to listen to John Kastelein’s interview with Petter Attia and he talks about this. And it makes sense since studies show poor correlation between LDL-C and ASCVD, meaning you can get ASCVD at both high and low levels and avoid it at high levels. So yes, there are all other risk factors, but still sometimes does not male sense. In some people there must be another protective mechanism that protects them from getting ASCVD and reverse cholesterol transport makes perfect sense to look at as lowering of LDL-C has just as much power as we know from RTCs. Even drastic lowering reduces absolute ASCVD mortality only marginally and data from prevention trials on healthy people is even more puzzling.
Thorin
#175
Regarding your side note: same. So far I have muted a total of one. I wonder how many have muted me? Probably more.
1 Like
Thorin
#176
The death from any cause graphic (bottom right) sure doesn’t look particularly compelling. And I say this as a person who is currently taking Rosuvastatin.
ng0rge
#177
Really! Who’d you mute?..just a test…to see if he hears me.
2 Likes
You ( (ng0rge) , Vlasko, and Thorin have muted the same individual.
My USD$50 goes to a charity of your choice if I am mistaken.
1 Like
Cholesterol Lowering, Cardiovascular Diseases, and the Rosuvastatin-JUPITER ControversyA Critical Reappraisal
Michel de Lorgeril, MD; Patricia Salen, BSc; John Abramson, MD; Sylvie Dodin, MD; Tomohito Hamazaki, PhD; Willy Kostucki, MD; Harumi Okuyama, PhD; Bruno Pavy, MD; Mikael Rabaeus, MD
Author Affiliations Article Information
Author Affiliations: Laboratoire Cœur and Nutrition, Faculty of Medicine, Université Joseph Fourier and Centre National de la Recherche Scientifique, Grenoble, France (Dr de Lorgeril and Ms Salen); Harvard Medical School, Boston, Massachusetts (Dr Abramson); Department of Obstetrics and Gynaecology, Laval University, Quebec City, Quebec, Canada (Dr Dodin); Department of Clinical Sciences, Institute of Natural Medicine, University of Toyama, Japan (Dr Hamazaki); Cardiology Department, Clinique Antoine Depage, Brussels, Belgium (Dr Kostucki); Open Research Center for Lipid Nutrition, Kinjo Gakuin University, Nagoya, Japan (Dr Okuyama); Réadaptation Cardiovasculaire, Centre Hospitalier de Machecoul, Machecoul, France (Dr Pavy); and Cardiology Department, Clinique de Genolier, Genolier, Switzerland (Dr Rabaeus).
ng0rge
#180
Who me? (what me worry?) I wouldn’t mute anybody…I rejoice in the whole spectrum of human idiosyncrasies. (and believe me you see 'em all here…not you, of course!)
P.S. I am just starting a charity tho.
1 Like
Okay. My mistake. Name your charity. I was serious about the USD$50.