Are there any issues with HDL being higher than LDL? My father’s latest results are a 34 LDL and 61 HDL. I thought I remembered reading somewhere that one being higher than the other is what is detrimental. Usually HDL is always lower than LDL.
Davin8r
#1060
Is high dose statin therapy also more anti-inflammatory then low dose statins, or is there an anti-inflammatory threshold that is met at lower doses? It’s too bad we don’t have a colchicine group (yet) to throw in there for comparison.
How do you measure “anti-inflammatory” in this context?
adssx
#1062
I don’t think anyone knows yet but the obicetrapib trials will help answer this question. My guess is that it’s okay or even protective.
1 Like
We do know that high HDL can be a negative, but anything in the 60 range is not “high”. Michael Lustgarten has a video somewhere, where he charts at which point HDL becomes a negative, and as I recall, the high end was above the 60’s, although surprisingly not much above 60’s already somewhere in the 70’s.
I am not aware of any data showing HDL higher than LDL being a negative. We can only speculate, and I too would speculate that it would be protective as long as the HDL is not crazy high; at 60-70, that’s not high. But speculation has little value, so ultimately we simply don’t know.
adssx
#1064
I don’t think we know that. There are probably many HDL subtypes with different effects. People who inhibit CETP live long and have low LDL and high HDL: Obicetrapib (CETP inhibitor for dyslipidemia)
2 Likes
That’s why I said “can” be a negative, there are many articles to that effect, and I have definitely heard Thomas Dayspring say so. That doesn’t mean high HDL is always a negative, for some subpopulations it may not… but then again, it’s the same with high LDL - high can be a negative, but not always, because there are documented sky high LDLs in FHC cases who have a normal lifespan with no medication, something in their physiology protects them. Lipids are complicated, full of special cases and exceptions, but general rules exist too. I myself on my last test had an HDL of 92mg/dL, LDL 133, and Lp(a) 78mg/dL (unfortunately, those are the units the lab uses) - and all of this on 10mg atorvastatin. Without the statin, my LDL was in the 180’s and HDLs often over 100. I’ve had very high cholesterol all my life. I’ve only been on a statin for 5 years. And yet, last December, I had a CAC scan, so age 65, and the score was stone cold ZERO. Now, maybe I have a ton of soft plaque, I don’t know, but the cardiologist thinks that’s unlikely and he discouraged an angio, which I wanted. I had a perfectly fine EKG, FWIW. Oh, also, the scan showed:
“The ascending aorta measures 29 mm, which is normal. No aortic valve leaflet calcifications. No atherosclerotic calcifications of the partially visualized thoracic aorta.”
The cardiologist said a 29mm aorta at my age and cholesterol levels is very good.
Point being: with lifelong terrible, unmedicated (until fairly recently) lipids, including high HDL and sky high Lp(a), at age 65, zero evidence of artherosclerosis (at least on a CAC scan). With these terrible numbers I was fully expecting extensive calcifications of my arteries. So: there’s general rules, but always exceptions.
3 Likes
adssx
#1066
“High HDL” is neither negative or positive, as of today, it’s just irrelevant:
And congrats on your 0 CAC score!
4 Likes
adssx
#1068
On plaque regression, does anyone understand his line of reasoning?
And commenting on this paper:
He said:

2 Likes
Stabilization is great. But wouldn’t regression after stabilization be even better?
2 Likes
On the one hand I can understand that if you have no MACE at a given level of plaque, then staying at that level, stabilizing, and NOT continuing the progession/increase in plaque deposits, you will continue to have no MACE. Mission accomplished: no MACE at this level? Maintain this level and continue to have no MACE.
But on the other hand, MACE cannot be the only criterion of CV health. If you have significant arterial stenosis (or vascular stenosis in general), then your CV system is performing subpar, and in time, you may in fact experience MACE (no MACE up to now doesn’t mean no MACE in the future), or a slow decline into heart failure, because stenosis is accompanied by high BP, which over time can lead to such outcomes, even at the same level of plaque. Time alone is a factor when your blood flow is obstructed and your heart has to work harder to pump blood through, leading to cardiac hypertrophy, pressure on arterial walls, rupture and so on, even if the plaque level is steady.
So intuitively, I’d think plaque regression would be a desirable outcome, as it could lead to improvements in other parameters, such as BP. Unless of course the plaque levels are very low, so there is no significant vascular stenosis, then ok, keep at that low level and you should remain fine. But hey, I’m not a lipidologist and Dayspring is, so he’s probably right for reasons I don’t understand.
4 Likes
mccoy
#1071
I should read Dr. Lipid’s words a few dozen times more, but after just 4 times I believe perhaps he says that there is not such a consolidated model of plaque regression, nor a consolidated treatment, so we should presently stick to the ascertained facts. “Regression is not necessary”. It may be useful though, It may help to decrease risk, but in the accepted model presently it’s not being modeled.
2 Likes
JKPrime
#1072
Makes sense. No doubt that very low levels of ldl-c will lower the cv risk and make you live longer, that said very low ldl-c may also increase your risk of dementia and who wants such a half-life?
1 Like
mccoy
#1073
Conceptually, we know that the brain does not need high systemic LDL-C. In the period when the central nervous system has its booming development, from fetus to toddler, LDL-C has trivial values around 20-30 mg/dL. The brain is a formidable synthesizer of its own cholesterol.
The concern, if I understood well, is the potential detrimental effect of statins on the synthesis of cholesterol in the brain. But nobody really knows, it is left to individual perception, like muscle aches. Brain fog after statins suggests discontinuation. And yes, genetic predisposition for dementia might suggest a precautional strategy of non-adoption of statins.
As far as logic and scientific evidence suggest, the narrative to keep LDL-C/ApoB as low as reasonably possible is totally founded.
The focus of the research now should be to provide the safest means (drugs) to execute this strategy.
4 Likes
adssx
#1074
The miracle threshold is apparently 5,000 mg/dL-years:
If this model is correct, then to be below the threshold for 100 years, you have to always be under 50 mg/dL.
You can calculate your long-term risk with this exposure calculator: https://dir.nhlbi.nih.gov/OCD/MultiRiskCVD/
4 Likes
mccoy
#1075
That’s pretty low, it corresponds to 131 mmol/lt -years, a value which I’m going to reach in 3 years and it’s not even a pessimistic estimate… 
By the way, cumulative exposure is very simple to calculate with a spreadsheet, you just draw a column for every year of life and for each single year you estimate, or report, your LDL-C in the same unit.
The sum of the values in the LDL-C column is the lifetime exposure.
4 Likes
mccoy
#1076
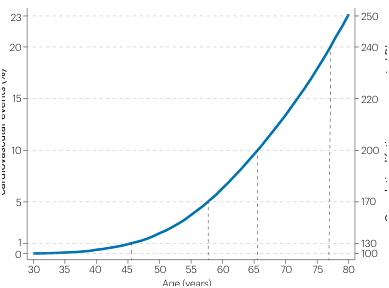
the 5000 mg/dL-year value is equal to the 1% cumulative risk value in the article by Ference et al., 2024, since this is the indicated (excess) lifetime risk at the value of 130 mmol/lt -years about equal to 5,000 mg/dL-years. This threshold in the UK biobank dataset is reached in men at 46 years of age (but their LDL-C values seem pretty high compared to other countries).
Again, this is a pretty low threshold, I wonder if it is too pessimistic, I’m going to listen to the video attentively
1 Like
A_User
#1077
Well, technically it’s possible to have a LDL below 10, just saying… If you stack all of the medications together and possibly have a very specific type of diet. PCSK9i + statin + ezetimibe + using canola oil instead of olive oil might be enough, and of course trying to decrease saturated fat as much as possible.
1 Like
mccoy
#1078
@AnUser If Kohsaka’s model is correct practically nuking LDL-C as you suggest wouldn’t be overkill. But again, it should be checked. If that’s true, after the age of 46 we should see an exponential rise in events in UK. Before taking such drastic measures I’m going to sit on the fence, meaning, I’m going to take less drastic measures…
By the way, I wasn’t able to find any relevant material from Dr Kohsaka